Abstract: During its five years of operations, Florida’s Medicaid Reform Pilot has been a decided success. It has improved the health of enrolled patients, achieved high patient satisfaction, and kept cost increases below average, saving Florida up to $161 million annually. Since then, Florida has passed its Statewide Reform, which promises to extend these benefits throughout the state, build on the lessons learned from the pilot program, and save up to $1.9 billion annually. If Florida’s Medicaid Reform Pilot experience were replicated nationwide, Medicaid patient satisfaction would soar, health outcomes would improve, and Medicaid programs could save up to $91 billion annually.
Numerous studies have shown that the best coverage for improving patient health is private insurance. However, in today’s health care marketplace, not everyone has access to private coverage, and the social safety net of Medicaid is provided to the truly needy and those with disabilities.
There are two models of health care reform that have fundamentally different approaches. One model empowers consumers to choose from among competitive, organized health plans based on measurable results important to the consumer. The second denies such freedom of choice to the consumer and instead relies on a centralized planning model in which government determines the type and scope of available health services and how service providers are compensated. Whichever model is chosen, the basic metrics for success are the same:
- Patient health is improved and continually improving,
- Patient satisfaction is high, and
- Cost increases are below average.
The goals of Florida’s Medicaid Reform Pilot, proposed in 2005 under then-Governor Jeb Bush, were the same: Improve key indicators known to coincide with good health, ensure that consumers are provided choices, achieve high consumer satisfaction, and keep cost increases below average. This paper examines how the Reform Pilot, now operating in five counties, has fared against these universal measures.
After five years, the evidence shows that Florida’s Medicaid Reform Pilot has:
- Maintained health outcomes at or above the national average for the majority of indicators and improved outcomes for recipients through financial incentives;
- Achieved patient satisfaction levels above the national averages of other state Medicaid programs and even commercial health maintenance organizations (HMOs); and
- Restrained costs, flattening the cost curve for per-person spending over the past five years.
The Reform Pilot’s fiscal impact has been significant, saving Florida Medicaid up to $161 million annually. If implemented statewide, it could reduce Medicaid spending by up to $1.9 billion annually. If Florida’s Reform Pilot experience were replicated nationwide, Medicaid patient satisfaction would soar, health outcomes would improve, and state Medicaid programs could save up to $91 billion annually.
The Florida Legislature has since passed the Statewide Reform, which would extend these Reform Pilot benefits to nearly all Florida Medicaid recipients. Implementation of the Statewide Reform is pending approval of several waivers by the federal Centers for Medicare and Medicaid Services (CMS).
A Tectonic Shift in Medicaid
Florida’s Medicaid Reform Pilot represents a fundamental shift in the state approach to Medicaid. For four decades, nearly every state has largely managed Medicaid through central planning, with states and the federal government directing which services would be provided, how those services would be delivered, and how costs would be paid. With the state at the center of the program, provider rates were dictated without regard to market conditions. This led to physician and provider shortages in specialties and failed to hold provider networks accountable for patient care. Scope of services and duration of benefits were based not on the patient’s needs, but in many cases on random budget decisions. The patient was nothing more than a passive participant. The cost of this runaway system was borne exclusively by the state and federal taxpayers.
Under Governor Bush, Florida advanced a new approach that prioritized the patient. From the outset, the Medicaid Reform Pilot was designed to be patient-centered. Patients would have a meaningful choice of multiple private plans, which offered varying sets of benefits and various provider networks. An innovative monetary rewards system would encourage and incentivize patients toward healthy, responsible behavior in managing and improving their own health. This was a tectonic shift away from central state management of individuals toward individuals managing their own care.
In addition, the Reform Pilot shifts risk. Taxpayers would no longer bear the financial risk of fraud and abuse or overutilization driven by unscrupulous providers. In the old system, the state simply paid claims, leaving taxpayers to pay hundreds of millions of dollars per year in fraud and abuse. Under the Bush plan, the private marketplace would absorb this risk as the state shifted to paying premiums rather than using the open-checkbook model of the fee-for-service system.
The premise was relatively simple. If the plans provided care management, limited provider network options to providers with the appropriate skills and reputations, and ensured that patients with chronic conditions received the tools to prevent the need for acute interventions, they would succeed financially. In terms of accountability, if plans provided unsatisfactory access to providers or in any other way did not meet the test for success, the consumer could switch plans, and the market would punish the plan.
In the Reform Pilot model, the state’s role would shift from being an active participant in the market to focusing more on ensuring that the market was working, regulating the plans, and measuring the outcomes of the system.
Under traditional Medicaid, patients have one alternative to becoming uninsured: Medicaid. Under the Medicaid Reform Pilot, the patient has the freedom and power to choose among many meaningful options. The patient, not politicians or bureaucrats, controls the money and chooses which plan, based on his or her needs and desires, receive the taxpayer dollars.
Florida’s Medicaid Reform Pilot tests four straightforward strategies to realize this patient-centered program for the low-income, disabled, and elderly populations:
- Give enrollees meaningful choices of customized managed care plans that can add benefits, limit certain optional services, vary copays (within federal limits) to promote consumer engagement in their care, limit or expand provider networks, customize drug formularies, and reward certain behaviors that lead to better health outcomes;
- Aggressively monitor patient health outcomes and satisfaction;
- Adjust managed care capitated rates through a risk-adjustment process based on health status to encourage appropriate care management; and
- Reward individuals with financial incentives to encourage responsible, healthy behavior.
The idea was that by implementing these four strategies, Florida’s Medicaid program would realize universal success in improved health outcomes and patient satisfaction for Medicaid enrollees and limit increases in Medicaid spending per enrollee for state taxpayers.
The idea sparked controversy because some opposed such extensive involvement by private managed care companies. Philosophically, these opponents prefer a one-size-fits-all government-run system even if it must work with private providers. Opponents did not believe that private managed care companies should be allowed to add or limit benefits, expand provider networks, revise drug formularies, or incentivize certain behavior. They thought this would be a backdoor to limiting services as a direct result of capping per-person payments to managed care plans.
In addition, many of these opponents draw political power from their ability to influence state Medicaid contracting and benefits. To surrender that authority to patients would be to cede their own political power.
Florida’s Medicaid Reform Pilot
The original legislation for the Reform Pilot passed with large bipartisan majorities of 39 to 1 in the Florida Senate and 88 to 24 in the Florida House.[1] The five-county pilot program covered the urban counties of Broward and Duval beginning in 2006 and rural counties of Baker, Clay, and Nassau, which surrounds Duval county, beginning in 2007. Participation was mandatory for low-income families and children and for those eligible for Medicaid who were receiving Supplemental Security Income (the elderly and those with disabilities). Enrollment was voluntary for other populations.
A Comprehensive, Diverse Pilot. These five counties have a diverse population of 2.93 million Floridians, a population greater than the population of 21 other states. Broward County, which includes Fort Lauderdale, has the same population as West Virginia. Today, 290,000 Medicaid recipients are part of the five-county Reform Pilot[2]—more individuals than the state Medicaid program in 17 states[3] and more than the entire Medicaid managed care populations in 28 states, including the 17 states with no comprehensive Medicaid managed care programs.[4]
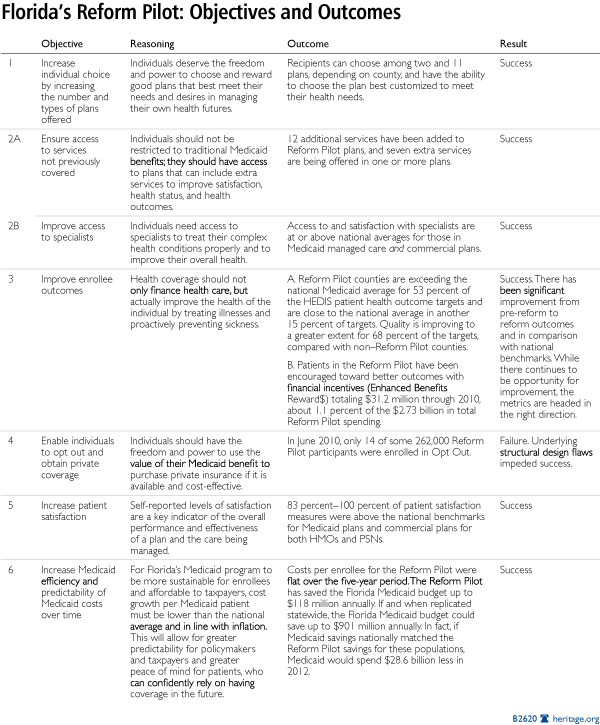
The Reform Pilot has five stated objectives:
- To increase the number of plans and enhance individual choice, including offering different types of plans;
- To ensure access to services not previously covered and improve access to specialists;
- To improve enrollee health outcomes;
- To enable individuals to opt out and obtain private coverage; and
- To increase patient satisfaction.[5]
This paper examines the actual outcomes for each of these five stated objectives, as well a desirable sixth objective:
- To increase Medicaid efficiency and stabilize costs over time.
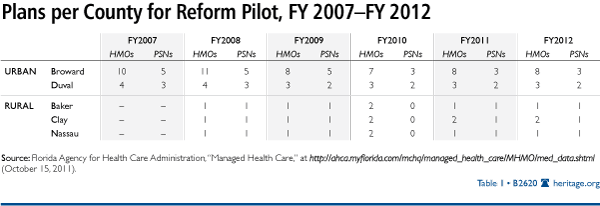
Objective 1: Increasing Individual Choice. Under the Reform Pilot, Medicaid patients were given a significantly larger number of plan choices. As Table 1 shows, the number of plans available to individuals in the Reform Pilot has been at least two and as many as 16 depending on the year and county. Recipients can choose between capitated managed care through HMOs or provider service networks (PSNs)—coordinated delivery networks more similar to managed care but with shared savings for the provider network rather than a pre-paid premium. In the rural counties with as few as 1,600 Medicaid recipients, individuals were offered a choice of two plans, the federal minimum for managed care.
The extent of choice in the Reform Pilot is impressive, particularly compared to the private sector and other state Medicaid managed care programs. The number of choices is more important for two primary reasons.
First, there are meaningful differences between the Reform Pilot plans making choice a substantive one.
Second, patients can reward or punish plans based on exercising their freedom to choose.
For comparison, only about half of Florida employees work in private companies that offer health insurance, are eligible for coverage, and can choose from more than one plan.[6] In Tennessee’s Medicaid program, the 1.6 million residents in mandatory comprehensive managed care can choose between only two managed care plans in each of the three regions.[7] In contrast, a Florida Reform Pilot region similar in size to a Tennessee region offers 11 plans.
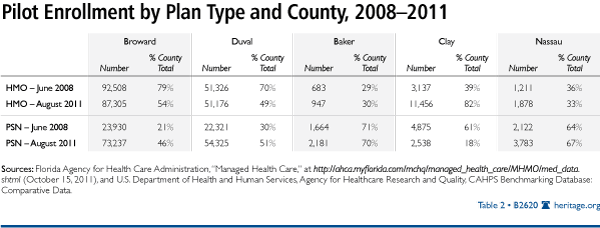
Medicaid patients have embraced this freedom of choice by making different choices over time, depending on their county of residence and their available options, as shown in Chart 1 and Table 2.
Some critics have claimed erroneously that beneficiaries are “moving in large numbers away from managed care to the PSN options available to them.”[8]
First, PSNs are managed care, just a model that is different from traditional HMOs. PSNs are provider-owned or provider-run networks, but PSNs still manage care and are still at-risk financially under Florida’s Reform Pilot PSN contracting structure.
Second, total HMO enrollment has remained relatively constant since 2008. However, aggregate enrollment in PSNs has grown, as shown in Chart 1. In some counties, the share of enrollees in PSNs has shrunk or remains flat. In other counties, it has grown. Clearly, individuals are voting with their feet—the entire point of freedom of choice.
By every measure, the choice strategy has been fully implemented. Medicaid patients have made varying choices over time, indicating both their interest and their eagerness to do so. This objective has been a success.
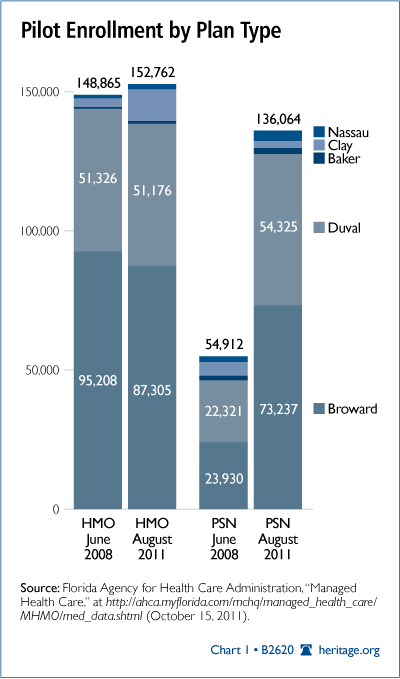
One measure of the real or perceived meaningfulness of plan choices is the portion of individuals who do not bother to select a plan and are simply automatically assigned to a plan. The higher the rate at which people are automatically assigned to a plan, the lower the perceived difference among plans.
In the Reform Pilot over the past several years, 70 percent to 80 percent of individuals have voluntarily selected their plans.[9] This puts the Florida Reform Pilot among the highest-performing Medicaid programs. For Florida’s non–Reform Pilot managed care counties, which is similar to traditional Medicaid managed care in most states, voluntary enrollment is at 60 percent.[10] In some states, only half, or as few as one-fifth, of individuals bother to select their managed care plans.[11]
Objective 2A: Ensuring Access to Additional Services. As part of their plan designs, HMOs and PSNs may offer additional services not typically covered by the traditional Florida Medicaid program. Over the past five years, they have offered as part of the Reform Pilot:
- Additional adult hearing benefits,
- Acupuncture,
- Additional hospital inpatient days covered,
- Additional hospital outpatient coverage, and
- Therapeutic massage.
For fiscal year (FY) 2012, at least one plan is offering:
- Over-the-counter drugs ($10 to $25 per household per month);
- Adult preventive dental;
- Circumcisions for male newborns;
- Additional adult vision benefits;
- Nutrition therapy and products, possibly including gym membership;
- Respite care; and
- Home-delivered meals following surgery.
People on Medicaid are no different from anyone else. Their plan choices should reflect their individual needs, wants, and situations. For example, in Broward County, only the South Florida Community Care Network plan offers a maternity benefit of home-delivered meals for families of newborns (two meals delivered for up to four people). This plan has a market share of 13 percent of all women ages 21–54 but 26 percent of all newborns.
These data suggest that South Florida Community Care is more attractive to pregnant women and has captured a greater market share because of the extra service targeted to expectant mothers.[12] Only one other plan offers an extra benefit targeted at newborns: Better Health offers circumcision coverage during an infant’s first three months.
Enrollees like extra benefits, and the more benefits a plan offers, the greater market share it has. In Broward County, the 44 percent of plans with the highest number of extra benefits (three or four) enroll 62 percent of recipients. Conversely, the plan that offers no extra benefits has only a 3 percent market share. Likewise, the one-third of plans that offer the highest range of hospitals in-network (13 to 15) enroll 41 percent of all recipients.[13]
In addition, plans may vary copays within allowable federal limits or waive copays entirely, and 80 percent of plans do not charge any copays.[14] Plans may also limit units of service covered and/or dollar benefits of certain Medicaid optional services. For example, plans for nondisabled parents and children have the following choices for benefits:
- Chiropractor (nine visits, 24 visits, or nine visits and $150 benefit);
- Dental (emergency and dentures only, $250 benefit, or $300 benefit);
- Durable medical ($250 benefit or other limits);
- Hearing (one device and one evaluation every three years or a $150 benefit per year);
- Home health (24 visits, 60 visits, or 10 visits and $200 benefit);
- Podiatrist (nine visits, 24 visits, or seven visits or $150 benefit); and
- Vision (one pair of glasses every two years or $150 benefit).[15]
The Reform Pilot also provides specialized packages. Positive Healthcare provides a customized plan for Medicaid patients with HIV+/AIDS. This plan offers $250 per year in nutritional products or gym membership, three hours per week of respite care, $1,000 annually for dental services, an unlimited pharmacy benefit, and higher durable medical equipment benefits.[16]
HIV+/AIDS patients need different benefits to manage their disease successfully. In Broward, the Reform Pilot plan offers them a plan tailored to their needs and condition. Whereas private individual insurance would often deny coverage to someone with HIV, the Reform Pilot welcomes them with a plan specifically tailored to their unique needs and with financial incentives to reward improved health outcomes.
As expected, Medicaid recipients respond favorably to extra services, more expansive hospital networks, and customized benefits. They like and select plans that offer them more options.
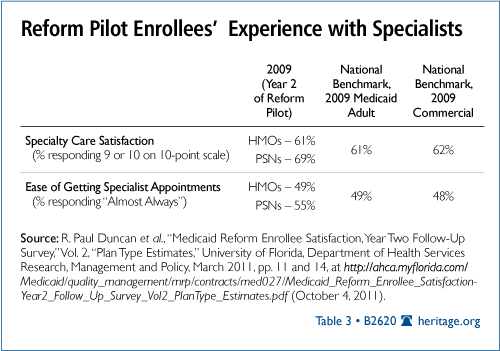
Objective 2B: Improving Access to Specialists. The Reform Pilot includes extensive client satisfaction surveys, which are administered by the University of Florida using the nationally recognized Consumer Assessment of Healthcare Providers and Systems (CAHPS) instrument. While the University of Florida has reported on the experiences of Reform Pilot recipients,[17] it has provided few details on how the results compare with national benchmarks for Medicaid managed care and commercial plans.
Table 3 shows the responses of those surveyed in Broward and Duval counties compared with national benchmarks taken directly from the Agency for Healthcare Research and Quality.[18] In both measures, Reform Pilot HMO enrollees report the quality and ease of access to specialists at the national average for both Medicaid and commercial plan recipients. Reform Pilot PSN enrollees reported quality and access to specialist care at far above the national averages for both Medicaid and commercial plan recipients.
Objective 3: Improving Enrollee Outcomes. The most universal measure of health plan enrollee outcomes is the National Committee for Quality Assurance’s Healthcare Effectiveness Data and Information Set (HEDIS), which is used by 90 percent of U.S. managed care health plans.[19] HEDIS measures are required in 25 state Medicaid programs.[20]
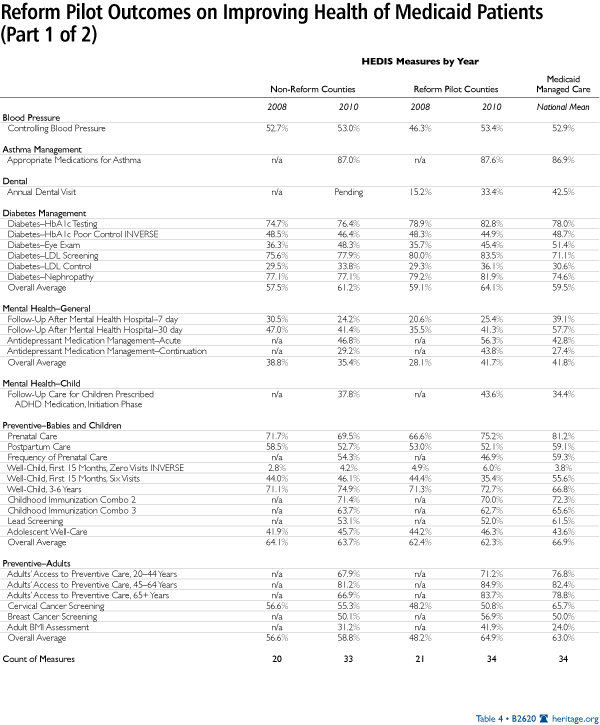
Table 4 shows the HEDIS outcomes for Reform Pilot counties compared to non–Reform Pilot counties and the national average for Medicaid HMOs for the most recent three years available.[21] On these enrollee health measures—including the four overall averages for diabetes, mental health, preventive-child, and preventive-adult measures—Reform Pilot counties outperformed non–Reform Pilot counties in 64 percent of the measures and exceeded the national average in 53 percent. For 68 percent of the measures, Reform Pilot counties showed greater improvement than non–Reform Pilot counties. In 78 percent, health outcomes improved in the Reform Pilot over the life of the measure. In another five measures (15 percent), Reform Pilot counties are within 5 percentage points of the national Medicaid average.
Clearly, more work can be done, but Reform Pilot counties are exceeding the national average in 53 percent of the HEDIS patient outcome measures and are near the national average in another 15 percent. In the aggregate, patients participating in the Reform Pilot are experiencing better health outcomes and greater improvements in health outcomes over time while exceeding the national average a majority of the time. This may not achieve the far-above-average ideal, but it is exceeding the benchmark.
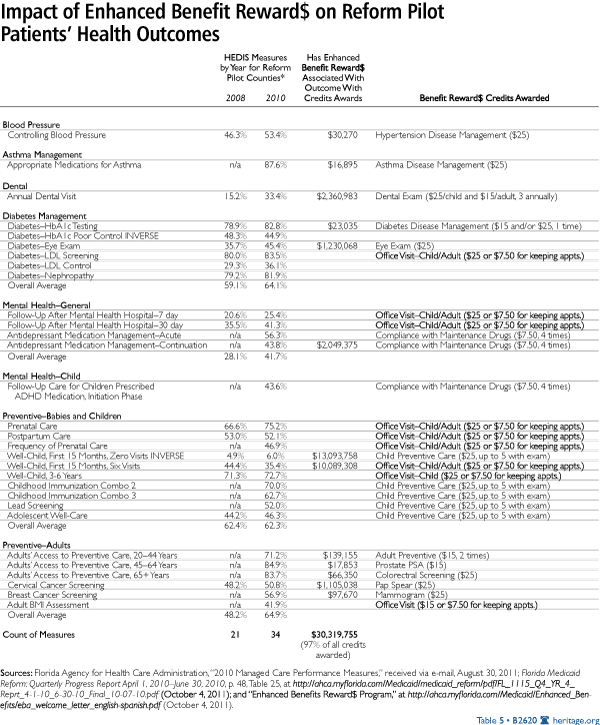
Another innovative feature of the Reform Pilot is the Enhanced Benefits Reward$ program, which gives financial rewards to individuals who receive certain preventive services, comply with maintenance and disease management programs, and keep appointments.
In the private sector, employers use wellness programs to encourage employees to take control of their own health status and to reduce the cost curve of private health insurance. Recent studies show the positive physical and fiscal impacts of promoting employee health and wellness. For example, employers with more than half of employees completing an adult health exam, health risk assessment, or biometric screening had a 1 percent to 1.5 percent lower cost trend compared with employers with low employee participation. As expected, increasing financial incentives dramatically increased participation in certain health risk assessments and other wellness programs. In addition, building a health-focused work culture and requiring participation in programs also increased employee participation.[22]
However, despite widespread use in large private companies’ health plans, state-run Medicaid programs have been very slow in adopting such best practices. Only West Virginia, Idaho, and Florida have adopted such practices in any significant way.[23]
- West Virginia required patients to participate in a wellness plan, undergo regular checkups, and listen to doctors’ orders to receive enhanced Medicaid benefits. However, West Virginia’s program was recently gutted due to changes in federal regulations prompted by passage of the Affordable Care Act.[24]
- In Idaho, children in the state’s Children’s Health Insurance Program (CHIP) who are up-to-date on their well-child visits receive a $30 credit per quarter. Credits can go toward monthly premiums for the CHIP program, which is $15 per month for a child in a family at 151 percent of poverty.[25] A recent study showed that the program has had a substantial impact in two years, increasing “the percentage of CHIP children who were up-to-date with well-child visits…by 116 percent (from 23 percent to 49 percent), compared with a 13 percent increase (from 29 percent to 32 percent) among children with Medicaid, who were not eligible for the incentive.”[26]
- In Florida, the Benefits Reward$ is one of the most prominent but least analyzed features of the Reform Pilot. In a typical month, 31,000–37,000 individuals were awarded credits. Through June 2010, $15 million of the $31 million awarded had been redeemed.[27] Individuals may earn up to $125 in credits per year for a variety of activities,[28] which are listed in Table 5.
Since the start of the Reform Pilot through FY 2010, $31.2 million has been awarded as Benefits Reward$. This represents about 1.1 percent of the $2.73 billion spent on Reform Pilot individuals. Individuals may use the Benefits Reward$ to purchase over-the-counter (OTC) items at pharmacies. Reward$ costs are built into the capitated rates and are not additional costs to the program. Most individuals use Benefits Reward$ to purchase child-rearing items such as diapers, OTC child medications, and similar child care items.[29]
The vast majority of the Benefits Reward$ measures encourage better outcomes, such as blood pressure management, asthma management, diabetes management, and preventive adult services. However, $23 million in Benefits Reward$ (almost three-fourths of all credits) has gone toward encouraging child preventive measures, which have been flat the past three years.
The Benefits Reward$ program is administered by the state and operates outside of the plan itself. Integrating it into and administering it through the managed care plan would seem to make more sense. It could then be tailored to the populations being served—such as those with HIV, the elderly, those with disabilities, children, and adults—and aligned with the other customized benefits and services. This integrated approach is used in the Statewide Reform.
Obtaining a better understanding of the impact of Benefit Reward$ in the Reform Pilot will ultimately require analysis similar to that completed in Idaho. By the same token, Idaho’s experience and Florida’s experience dramatically show the power of a Reward$-type program, which costs little (1 percent) but can dramatically improve vital health behaviors.
Objective 4: Opting Out of Medicaid and Choosing Private Coverage. The Reform Pilot allows individuals to opt out of Medicaid and, when available and cost-effective for the state, to use the dollar value of their Medicaid benefits to pay the employees’ share of the premium for family coverage provided through their employers. This option is important as patients with private coverage repeatedly have been shown to have better health outcomes than those with Medicaid or the uninsured.[30] Thus, the best option is private coverage, with the second-best being the best-designed, personalized Medicaid plan.
At the end of FY 2010, only 14 individuals were enrolled in the Opt-Out program, and 75 individuals had enrolled in the benefit.[31] A 2008 report from the Florida Legislature’s Office of Program Policy Analysis and Government Accountability noted that only 91 individuals expressed interest in the Opt-Out program during the first 18 months. Of these, 15 were ineligible, 59 choose not to participate, and 17 enrolled their families, for a total of 30 enrollees.[32] Therefore, about 22 percent of those eligible and referred to the program enrolled. Yet by any measure, participation has been extremely small.
In 2010, the U.S. Government Accountability Office reported on enrollment in state Medicaid premium assistance programs (similar to Opt-Out) in 39 states as of June 2009. Florida had the seventh-lowest number of enrolled individuals (21) of any state despite having the fourth-largest Medicaid program.[33] For the 32 states reporting enrollment, just 0.28 percent of child and adult Medicaid enrollees were enrolled in these premium assistance programs, or Opt-Out. However, the portions of individuals in premium assistance varied dramatically from 0.00 percent in Florida to 6.5 percent in Rhode Island.[34]
The characteristics of successful programs show that Florida could improve and expand Opt-Out by:
- Making private coverage mandatory if cost-effective. If the private insurance option is mandatory, enrollment is six times higher (1.9 percent) than if it is voluntary (0.3 percent).
- Including non-group (individual) health insurance. Half of the top-performing states (more than 2 percent enrolled) included non-group coverage.
- Offering Opt-Out to both Medicaid and CHIP enrollees. States offering options in both programs averaged 8 percent higher enrollment in Medicaid, possibly the result of children moving between Medicaid and CHIP premium assistance based on family income.
Certainly, higher-income limits on Medicaid eligibility affect the enrollment in premium assistance because those with higher incomes are more likely to have access to employer-sponsored coverage. However, even for states with Medicaid income limits similar to Florida’s, 0.3 percent of all children and adults in Medicaid are enrolled in premium assistance. For example, Texas had about 3 million people in Medicaid in June 2009 compared to 2.5 million in Florida, yet Texas had 8,671 individuals in premium assistance compared to just 21 in Florida.[35] To reach the 0.3 percent threshold, Florida would need to enroll 5,900 people.
From the Reform Pilot experience, Florida needed to revamp and expand Opt-Out and replicate the success of other states. However, Florida also should consider rebranding the program from Opt-Out to Private Insurance Option to reflect more accurately that individuals are receiving coverage through private insurance with Medicaid paying the premium, not opting out of coverage altogether.
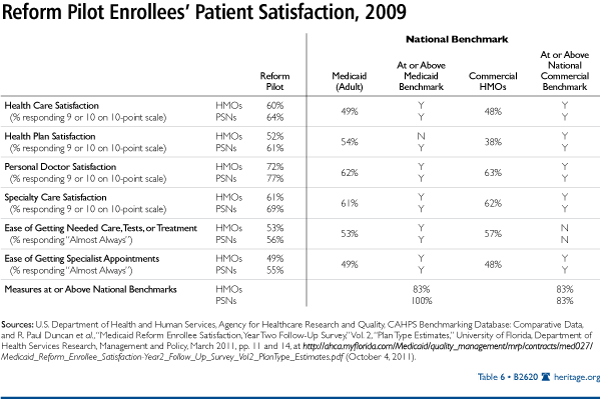
Objective 5: Increasing Patient Satisfaction. Despite spending hundreds of billions of dollars annually, Medicaid tracks enrollee satisfaction only to a limited degree. The most nationally recognized instrument is the Consumer Assessment of Healthcare Providers and Systems conducted by the Agency for Healthcare Research and Quality in the U.S. Department of Health and Human Services. In 2009, the most recent year for which state and national results are publicly available, Florida was one of 12 states with Medicaid programs participating in and reporting results to the national CAHPS Benchmarking Database. Florida had 13 Medicaid managed care plans participating, the second-highest of any state, constituting more than one-tenth of the 126 Medicaid managed care plans reporting for adults.[36]
For Reform Pilot HMO plans, 83 percent of measures were at or above the national Medicaid benchmark and at or above the national commercial plan benchmarks.[37] For Reform Pilot PSNs, all measures were at or above the national Medicaid benchmark, and 83 percent were at or above the national commercial plan benchmarks.[38] (See Table 6.)
Objective 6: Increasing Efficiency and Cost Predictability. Florida’s Reform Pilot has produced health outcomes that are at the national average for Medicaid managed care programs and that—most important—are improving. In addition, the Reform Pilot has produced patient satisfaction levels above the national average for both Medicaid managed care and commercial HMOs. The Reform Pilot has given individuals meaningful choices, and individuals are clearly using that freedom and power in choosing (and rewarding) good plans and selecting the doctors and hospital networks that best meet their needs and desires. Individuals are also being financially rewarded for making wise choices in managing their health futures and in following chronic care guidelines.
How has the Reform Pilot performed financially in comparison with the overall averages for Florida and the U.S.? The two key data sources in answering this question are the capitated HMO rates for the Reform Pilot’s two contract regions (Broward and Duval with the three adjacent rural counties combined) and the recorded spending for similar Medicaid populations according to the U.S. Department of Health and Human Services’ Centers for Medicare and Medicaid Services’ Medicaid Statistical Information System (MSIS) dataset.[39]
In the Reform Pilot, HMOs are paid a capitated flat, fixed monthly rate for all individuals over one year old. Different rates apply for children under three months old and children between three months and 12 months. Although PSNs have a different contract arrangement, they are required to meet similar financial benchmarks. In Florida, the current set of HMO contract rates is approved through August 2012, providing longer-term comparison.
These Reform Pilot capitated rates are then risk-adjusted based on each individual’s health status. In Florida’s non-Reform managed care, rates are varied based on age, gender, category of Medicaid eligibility, and geography and are not risk-adjusted for health status.[40] With the Reform Pilot’s risk adjustment for health status, managed care companies have a strong financial incentive to enroll sicker patients and effectively coordinate their care and improve those patients’ health.
Given the superior fiscal performance of the Reform Pilot, as shown below, and the superior health outcomes of Reform Pilot patients, the health-based risk-adjustment process is clearly achieving its desired goals. That is good for everyone—Medicaid patients, taxpayers, and the managed care companies. And that is likely why two-thirds of Medicaid managed care programs nationwide risk-adjust their rates based on health status.[41]
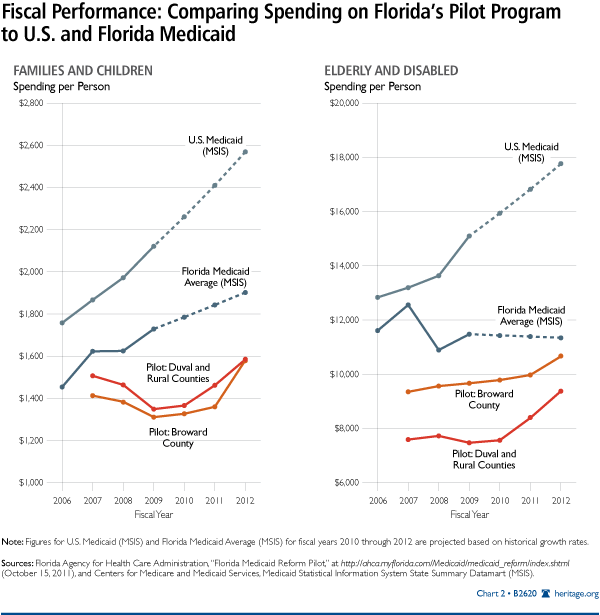
Using the Reform Pilot HMO contracts and the MSIS dataset,[42] Charts 3 and 4 show the fiscal performance of the Reform Pilot compared with the average spending for a population similar to the population of Florida and for the U.S. population for individuals more than one year old. The U.S. and Florida Medicaid spending per person for FY 2010 through FY 2012 is projected based on the historical annual growth rates for each category from 2007 through 2009 as calculated from the MSIS dataset.
In all cases, the Reform Pilot has a much lower growth rate than the U.S. or Florida averages. For 2007 through 2009, for which there are directly comparable data, per-person Medicaid spending for Temporary Assistance for Needy Families (TANF) children and adults grew 12.0 percent nationally and 6.1 percent in Florida but dropped 11.7 percent in Duval and the rural counties and 7.8 percent in Broward county. Per-person Medicaid spending for the Supplemental Security Income (SSI) elderly and disabled grew 12.6 percent nationally; dropped 9.4 percent in Florida overall; dropped slightly in Duval and the rural counties (1.6 percent); and increased slightly in Broward (3.3 percent). In both groups, the Reform Pilot cost much less than the U.S. Medicaid average.
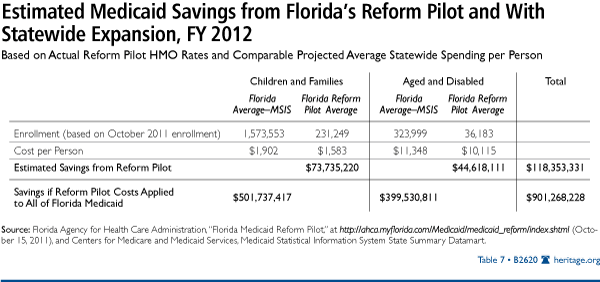
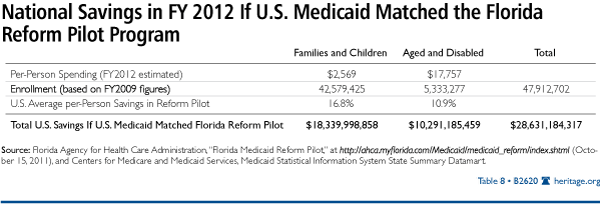
In fact, if Medicaid spending nationally matched the Reform Pilot costs for these populations, Medicaid would have spent $68.5 billion less in 2009 and would spend $91.1 billion less in 2011. The federal government would benefit from about 57 percent of those savings ($39 billion in 2009 and $52 billion in 2011),[43] with the rest going to state budgets ($29.4 billion in 2009 and $39.2 billion in 2011), as shown in Table 7.
Florida’s Reform Pilot has produced real savings to the state Medicaid budget. Based on enrollment figures for June 2009 and average spending per person from the MSIS data for Florida, the Reform Pilot has saved the Medicaid budget up to $161.6 million annually. If and when replicated statewide, the Florida Medicaid budget could save up to $1.9 billion annually, as shown in Table 8.
2011 Statewide Medicaid Managed Care
Based on the successes of the Reform Pilot and the lessons learned over the past five years, the Florida Legislature passed and Governor Rick Scott signed legislation in spring 2011 to apply the lessons learned from the Reform Pilot in creating the new Statewide Reform program. The Statewide Reform applies five lessons from the Reform Pilot.
Lesson #1: Copy what works.
Policy: Expand mandatory participation beyond the poor, elderly, and physically disabled.
The Statewide Reform expands mandatory managed care beyond the individuals in the Reform Pilot to include medically needy individuals on Medicaid. Those with developmental disabilities, participating in home and community-based services waivers, or in certain mental health or juvenile justice institutions are excluded from mandatory managed care under the statewide expansion.
Lesson #2: Proactive steps are needed to increase rural plan choices.
Policy: Create incentives to expand access in rural areas.
One lesson learned from the Reform Pilot is to create multicounty regions that have a critical mass large enough to attract a significant number of plans and that added incentives are needed to support multiple plans in certain less populated, rural regions. For example, the four smallest Reform Pilot counties are included in the broader Region 4.
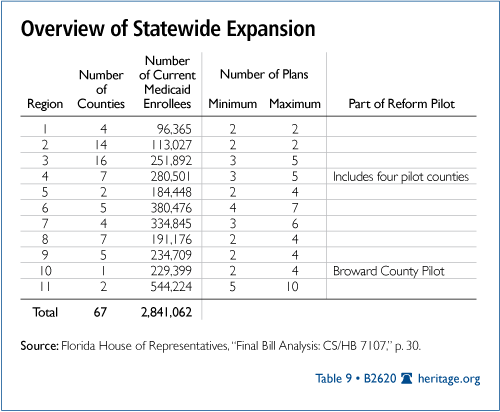
To ensure an adequate number of plans in rural areas, the legislature divided Florida’s 67 counties into 11 regions with five-year plan contracts. Each of the regions has a minimum of two plans, including one PSN, and a maximum of between two and 10.[44]
Region 1 (four counties) and Region 2 (14 counties) are in Florida’s rural panhandle and can have a minimum and maximum of two plans each. To encourage participation in these rural counties, plans that bid successfully in either region are given the choice of another region in which that plan would receive a guaranteed contract, assuming that it bid on that other region and charges an acceptable rate. However, if that plan terminates its contract in Region 1 or Region 2, it automatically loses its additional region.[45] Thus, winning in the rural panhandle is a guaranteed gateway to winning in a larger, more densely populated region of the state.
Lesson #3: Medical liability costs affect patient access to providers.
Policy: Lower the cap on noneconomic medical malpractice damages for providers when treating Medicaid patients.
To encourage access to providers, the Statewide Expansion legislation lowers the cap on noneconomic damages for providers treating Medicaid patients. In 2003, the legislature capped noneconomic damages at $500,000 for doctors and $750,000 for hospitals to reduce medical malpractice expenses. As Table 9 shows, it worked. Premiums dropped 36 percent due to lower payouts and fewer cases.
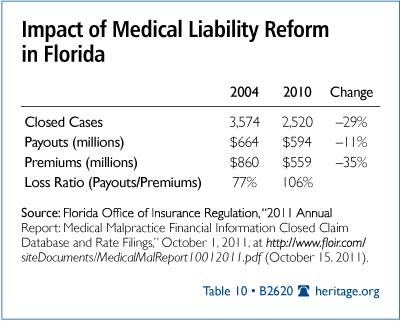
The Statewide Reform builds on this medical malpractice reform by reducing the cap on noneconomic damages for Medicaid patients to $200,000 for individuals and $300,000 per incident. Combined with increases in physician reimbursement, this additional malpractice reform should increase access by reducing the cost of treating Medicaid patients.
Lesson #4: Greater accountability and transparency for plans is better for patients.
Policy: Change the contracting process and patient disclosure to further improve patient satisfaction.
The Reform Pilot showed the importance and impact of tracking patient satisfaction and health outcomes—something too few states do even now. Building on this, the Statewide Reform requires plans that are awarded contracts for each region to maintain those contracts, absent gross negligent behavior, for five years. This provides continuity for patients and encourages long-term provider contracting and better networks for patients. In addition, plans are required to increase reimbursement to physicians, matching Medicare rates, to expand access; host online the listing of the prescription drug formulary; accept prior authorization requests electronically; have adequacy standards for provider networks; publish quality data measures online; and host an up-to-date online service that shows patients the physicians, specialists, other health providers, and hospitals in their networks, as well as whether or not they are accepting new patients and their contact information and working hours.
Despite the five-year contract, plans may alter their benefits, add extra benefits, or make other benefit changes annually. Individuals may also change plans annually or at a qualifying event, thus maintaining choice and plan customization and specialization.
Lesson #5: Link Benefits Reward$ to the plan and make it patient-centered.
Policy: Customize and tailor Benefits Reward$ to match plan design and patient needs.
One-size-fits-all does not work for Benefits Reward$. The Statewide Reform changes administration of the Benefits Reward$ and allows the plan to customize the program to align best with the plan designs and patient populations.
The current Reward$ program is not as effective and efficient as it could be. Although those with HIV have a customized plan, only one Reward$ category specifically targets this population. Obviously, a Reward$ program for those with HIV should be dramatically different from one for infants in need of extensive preventive care and immunizations. The Statewide Reform recognizes this and makes this important change. This change will also allow plans to monitor and publicly report how the Reward$ program is helping their patients and improving their patients’ health outcomes.
Additional Policy Recommendations
The Statewide Reform does not include all of the policy recommendations resulting from this analysis of the Reform Pilot and the key lessons learned. As the legislature fine-tunes the Statewide Reform, it should consider:
- Encouraging at least three plan choices in each region and combining regions if necessary to achieve this level of choice. A ceiling or floor of only two plans for a region, as required by federal law, undermines the point and innovation of the Reform Pilot. The Reform Pilot has shown that some rural counties and regions are too small for extensive choices. In the Statewide Expansion, all regions should be large enough to support a minimum of three or, ideally, four plans to create choices that have meaningful distinctions in benefits and networks.
- Fixing Opt-Out by copying successful premium assistance programs in other states. The Reform Pilot showed how not to run premium assistance. Although the legislature made some of these changes in the enabling legislation, such as including non-group health plans, the Statewide Reform as currently planned maintains too many features of the unsuccessful program in its current form. Florida should fix Opt-Out by making private coverage mandatory if cost-effective, expanding premium assistance to CHIP, and rebranding it as the Private Insurance Option.
- Studying whether to expand Statewide Reform to include children covered by CHIP. The Reform Pilot was not available to CHIP children. However, given the success of the Reform Pilot, expanding Statewide Reform to include this population and tailoring it accordingly could make sense. Plans could copy Idaho by using Reward$ for the CHIP to offset any monthly premiums charged to families. In addition, CHIP children and their parents could then have the same freedom and power to choose that those in the Statewide Reform have.
Conclusion
Florida’s Medicaid Reform Pilot is one of the most comprehensive, innovative, and significant Medicaid reforms of the past decade. It has improved health, produced high patient satisfaction, and dramatically flattened the Medicaid cost curve. The Florida Legislature and Governor Scott wisely built on the Reform Pilot to create Statewide Reform, which will allow all Florida Medicaid recipients to benefit from this improved, patient-centered Medicaid program. A few additional reforms would improve the Statewide Reform even further.
Implementation of Florida’s Statewide Reform cannot take effect unless the CMS approves several waivers. As the CMS reviews the waiver applications, it should note the huge success of the Reform Pilot and the key lessons learned that have been built into the proposed Statewide Expansion.
Other states seeking to improve health, increase satisfaction, and control costs should consider replicating Florida’s reforms. If the results of Florida’s Reform Pilot were replicated nationwide, Medicaid patient satisfaction would soar, health outcomes would improve, and Medicaid programs could save up to $91 billion annually.
Not only should the CMS approve Florida’s Statewide Reform waivers, but the Obama Administration should use its bully pulpit to encourage other states to replicate Florida’s experience to improve Medicaid for both patients and the taxpayers.
—Tarren Bragdon is President and CEO of the Foundation for Government Accountability, a free-market think tank in Naples, Florida.
Appendix
Methodology for Fiscal Analysis
Enrollment
Enrollment for FY 2012 was based on the Florida Agency for Health Care Administration’s October 2011 Comprehensive Managed Care Enrollment report.[46]
Families and Children (TANF). Reform Pilot Enrollment was based on the TANF enrollment for those in Reform Pilot counties and over age 1 (245,494 – 14,245 (under 1 year old) = 231,249).[47]
Statewide TANF Medicaid enrollment was based on the TANF enrollment in non–Reform Pilot counties[48] (1,670,438) and adjusted based on the assumption that a similar portion of TANF enrollees in non–Reform Pilot counties were over age 1 as in Reform Pilot counties (231,249/245,494 = 94.2%) for an estimated statewide non–Reform Pilot TANF enrollment of 1,573,553 (1,670,438 * 94.2%).
Elderly and Disabled (SSI). Reform Pilot enrollment was based on the SSI enrollment of those in Reform Pilot counties, over age 1, and not on Medicare[49] (36,370—187 (under 1 year old) = 36,183).
Statewide SSI Medicaid enrollment was based on the SSI enrollment in non–Reform Pilot counties[50] (325,627) and adjusted based on the assumption that the portion of SSI enrollees in non–Reform Pilot counties over age 1 was similar to the portion in Reform Pilot counties (36,183/36,370 = 99.5%). This yielded an estimated statewide non–Reform Pilot SSI enrollment of 323,999 (325,627 * 99.5%).
Per-Person Costs
Per-person costs for FY 2012 were based on the Florida Agency for Health Care tAdministration’s composite monthly HMO capitated rate for Reform Pilot enrollees[51] and a projection for 2012, which was based on historical average annual growth of actual spending for similar populations in the CMS Medicaid Statistical Information System[52] for Florida and the U.S. as a whole in 2009.
Families and Children (TANF). Reform Pilot annual Medicaid per-person costs were based on the weighted average, which was based on enrollment of the FY 2012 TANF HMO capitated rate for those in the Reform Pilot counties over age 1 ($131.78 per month in Broward County and $132.09 per month in the other Reform counties).[53]
Statewide Florida TANF Medicaid per-person costs were based on MSIS spending for a population comparable to the Reform Pilot TANF over age 1 for FY 2006–FY 2009.[54] Costs were projected to 2012, based on the historical growth rate of per-person spending from 2007, when the Reform Pilot began, to 2009, the most recent year for which data were available.
The United States average for TANF Medicaid per-person costs was based on MSIS spending for a population comparable to the Florida Reform Pilot TANF over age 1 for FY 2006–FY 2009.[55] Costs were projected to 2012, based on the historical growth rate of per-person spending from 2007 to 2009, the most recent year for which data were available.
Elderly and Disabled (SSI). Reform Pilot annual Medicaid per-person costs were based on the weighted average, based on enrollment of the FY 2012 SSI HMO capitated rate for those in the Reform Pilot counties over age 1 and not on Medicare ($888.25 per month in Broward County and $781.40 per month in the other Reform Pilot counties).[56]
Statewide Florida SSI Medicaid per-person costs were based on the MSIS spending for a population comparable to the Reform Pilot TANF over age 1 for FY 2006–FY 2009.[57] Costs were projected to 2012, based on the historical growth rate of per-person spending from 2006 to 2009, the most recent year for which data were available.
The U.S. average for SSI Medicaid per-person costs were based on the MSIS spending for a population comparable to the Florida Reform Pilot SSI over age 1 for FY 2006–FY 2009.[58] Costs were projected to 2012, based on the historical growth rate of per-person spending from 2006 to 2009, the most recent year for which data were available.