Both the House and Senate health care bills would increase health insurance coverage principally by expanding the federal–state Medicaid program. In fact, depending on the version enacted, the Medicaid expansion would account for between three-fifths and four-fifths of the projected reduction in the uninsured population under the legislation.
While the national debate over the cost of these bills has focused largely on their federal budget implications, their Medicaid expansion provisions would also impose significant additional costs on state government budgets and state taxpayers. Not surprisingly, governors and state legislators—from both parties and across the country—are objecting to the added costs that these bills would impose on their states. Their concerns are genuine and justified.[1]
Hidden Expenses
Both bills attempt to address state concerns by having the federal government pay for a large share of the expansion costs.
Under the House bill, the federal government would pay all of the benefit costs for the expansion in the first two fiscal years (FY 2013 and FY 2014) and then 91 percent of the benefit costs in subsequent years. The Senate bill would pay for all of the benefit costs for the expansion in the first three calendar years (2014 through 2016) and then between 81 percent and 95 percent (depending on each state’s match rate) in subsequent years.
However, even with the enhanced federal match rates, states would still face significant additional Medicaid costs.
Added Administrative Costs
Furthermore, beyond the benefit costs of the expansion, there would be significant additional administrative costs—which are not included in the official estimates—to both the federal and state governments.
Administrative costs are divided between the state and federal governments at separate, uniform match rates. The standard administrative cost match rate is 50 percent, though the federal government provides higher match rates for a few, specified administrative expense items.
The most recent available Medicaid expenditure data (for federal FY 2006 and 2007) show that administrative expenses add an average of 5.5 percent on top of total (federal and state) benefit costs and that, on average, the federal government pays 55 percent of total administrative costs, with the other 45 percent paid by the states.[2] Because neither bill changes the match rates for administrative costs, this additional state spending on administrative costs will occur even if the federal government pays 100 percent of the added benefit costs.
Just the state share of administrative costs for the benefit expansion is projected to be $9.6 billion for FY 2014 to FY 2019 under the Senate bill and $14 billion for FY 2013 to FY 2019 under the House bill. Indeed, the state share of administrative costs for the expansions would exceed $100 million a year in each of the four biggest states (California, Florida, New York, and Texas) and, under the House bill, is projected to cost California over $385 million a year by FY 2019.
Cost Burden on States
Calculations of state costs, derived from the coverage and federal cost estimates prepared by the Centers for Medicare and Medicaid Services (CMS), show that the Senate bill would increase state Medicaid spending—for both benefits and administration—by $32.6 billion for FY 2014 to FY 2019, while the increased Medicaid costs to states under the House bill would be $60 billion for FY 2013 to FY 2019.[3]
Table 1 summarizes the federal and state Medicaid costs under the two bills.
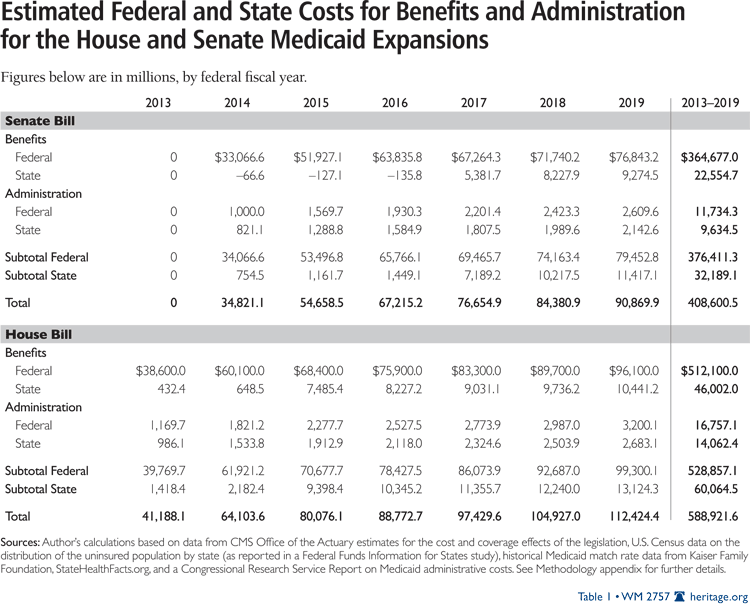
The Medicaid expansion is bigger in the House bill than in the Senate bill. The House bill would expand Medicaid up to 150 percent of the federal poverty level (FPL), while the Senate bill would expand coverage up to 133 percent of FPL. In the House bill, the expansion provisions would take effect in 2013; in the Senate bill, they would start a year later.
In addition, the House bill (but not the Senate bill) would require states to provide Medicaid “wrap-around” coverage to Medicare beneficiaries between 100 percent and 150 percent of FPL—at standard match rates.
Table 2 provides estimates of state spending for each of the 50 states and the District of Columbia under the Senate and House bills, respectively.
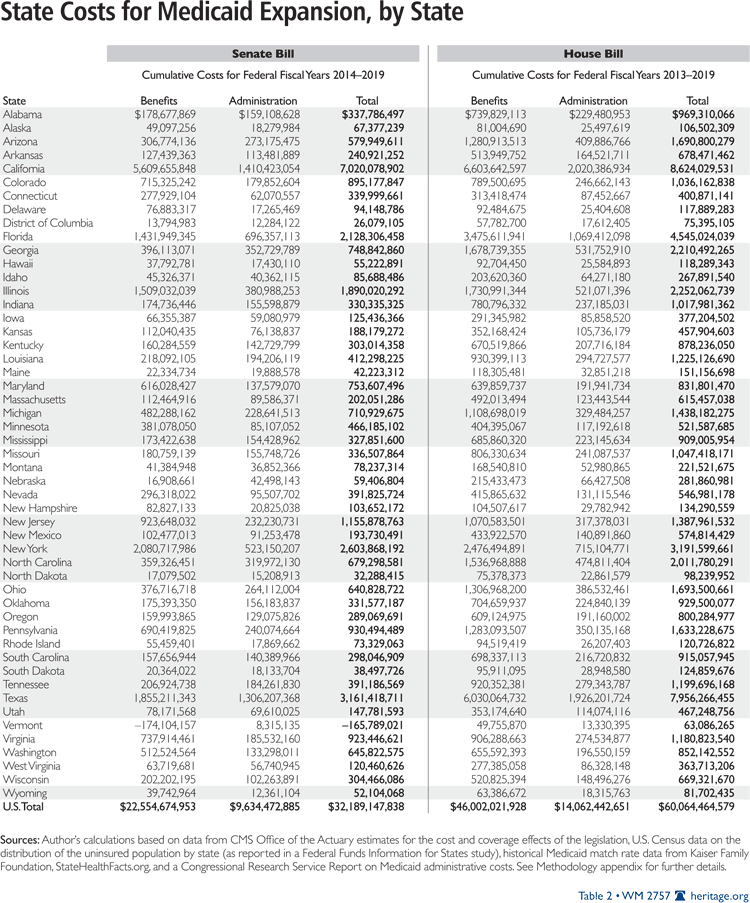
The Senate Medicaid Special Deals
The last-minute inclusion in the Senate bill of provisions giving three states special Medicaid funding deals has generated considerable attention and controversy.[4] Table 3 projects the savings to the three states from their special Medicaid funding deals.

Massachusetts and Vermont were given temporary increases in their federal matching rates for spending on their existing Medicaid populations for periods of three and five fiscal years, respectively.[5] The rationale offered is that those states have already expanded Medicaid coverage above the levels specified in the Senate bill and thus would incur few or no new costs as a result of the expansion.
While some might consider it illogical that extra federal funding should be earmarked for two states on the grounds that they need it the least, it is likely that the authors of these deals view the extra federal payments as “rewards” to those states for having already imposed on their taxpayers the burdens that Congress intends to impose on the other 48 states.
It was, however, the Senate leadership’s offer to pay all of Nebraska’s added benefit costs for the Medicaid expansion that sparked the most controversy, with lawmakers in other states demanding similar deals. In fact, due to the way that provision was drafted, Nebraska will actually have to pay its share of the benefit cost for the expansion in FY 2017—estimated at $16.9 million—with the exemption then applying in FY 2018 and beyond. Of course, as with all other states, Nebraska will still be responsible for paying its share of the extra administrative costs starting in 2014 when the expansion takes effect. Nebraska’s extra administrative cost over the period FY 2014 to FY 2019 would be an additional $42.5 million burden on Nebraska taxpayers.
Effect of Expanding the “Nebraska Exemption”
As Table 1 shows, expanding the “Nebraska exemption” by having the federal government also relieve all of the other states of all of their remaining benefit costs for the Medicaid expansion would add another $23 billion to the federal 10-year cost for the Senate bill, or another $46 billion to the federal cost for the House bill, while still leaving states responsible for funding their share of administrative costs.
Washington ’s Solution: Punt It to the States
Hiding behind all the costs, complexity, bureaucracy, and disruptions that these massive bills would impose on Americans who already have health insurance can be found this Congress’s principal solution to the problem of uninsurance: Dump the vast majority of the uninsured into Medicaid, leave the states with the messy job of trying to make it work, and give states just enough in extra transfer payments to buy off opposition until enactment.
It is neither an edifying spectacle nor good health policy.
Edmund F. Haislmaier is Senior Research Fellow in the Center for Health Policy Studies at The Heritage Foundation.
Appendix: Methodology
State-level estimates were generated by using the CMS Actuary’s estimates for the effect of the Medicaid expansions on enrollment at the national level and on federal Medicaid spending to derive the average federal cost per enrollee per year and by using the distribution of the uninsured population by income among the various states as a proxy for the distribution of the population that would be newly enrolled under the expansion provisions.
For example, if today a particular state accounts for, say, 1.2 percent of all uninsured Americans below 133 percent of FPL, then it is assumed that the state will also have a 1.2 percent share of the total new Medicaid enrollment under the Senate bill. Multiplying the projected per-capita federal cost by the number of projected enrollees in a state gives the portion of federal benefit spending that will flow to that state. The state costs are then calculated off the federal cost estimates by using the applicable match rates for each state as adjusted by the provisions of the legislation.
The added administrative cost load was calculated by applying current ratios for total administrative costs as a percent of total benefit spending and then apportioning those costs between the federal and state governments based on historical data that indicate an average effective Federal Medical Assistance Percentage (FMAP) of 55 percent for all administrative costs.
These state-level estimates should be treated as approximate. State officials will likely be able to construct more precise estimates for their own states using their own coverage and Medicaid program data—data that are not easily available to external researchers.
In general, basing these estimates on the CMS projections implicitly incorporates into them the underlying CMS assumptions for future population and spending growth rates. Using CPS data on the uninsured as a proxy for distributing the expansion population across the states should capture most of the differences among states in their current program eligibility levels.
That is, if two states have about the same total population but the uninsured rate is higher in one than the other, it is likely that at least part of that difference can be explained by differences in the two states’ Medicaid eligibility criteria for non-elderly, non-disabled adults as well as any other Medicaid waiver or state-only program targeted to that population.
However, one uncertainty is the extent to which the uninsured population of a given state consists of illegal immigrants, who would be barred from obtaining coverage through Medicaid. Estimates for the share of the national uninsured population that consists of illegal immigrants are imprecise, and attempting to adjust for the presumed uneven distribution of that subpopulation across the states would be even more problematic.
Moreover, reliable state-level data, consistent across all states, for per-capita Medicaid spending for the subset of current beneficiaries who most closely match the characteristics of the expansion population are not readily available. However, each state’s program officials should be able to use their own state’s Medicaid data to project their own costs.
Thus, a major limitation of this set of state-level estimates is the need to assume the same per-capita spending amount for new enrollees across all the states. The inability to incorporate state-level spending variations into these estimates is likely to be a major explanation for any variance between these estimates and a state’s own calculations.
Components and Data Sources
Enrollment and Federal Spending. CMS projections as found in Tables 1 and 2 of the CMS Actuary’s memos entitled “Estimated Financial Effects of the ‘America’s Affordable Health Choices Act of 2009,’ as Passed by the House on November 7, 2009” (November 13, 2009) and “Estimated Financial Effects of the ‘Patient Protection and Affordable Care Act of 2009” (December 2009).
CMS projections were used instead of the equivalent CBO projections because CBO implicitly assumes that this expansion would follow the observed pattern of previous expansions, with enrollment growing gradually over a period of years as newly eligible individuals sought assistance or were identified through outreach efforts. In contrast, CMS explicitly (and more plausibly) assumes that other provisions of the legislation—specifically, the individual mandate, the additional eligibility determinations to be conducted by the new exchanges for a much larger population that might be eligible for new subsidies outside of Medicaid, and the Medicaid automatic enrollment provisions—“would result in a high percentage of eligible persons becoming enrolled in Medicaid” and that “the great majority of such persons would become covered in the first year, with the rest covered by [the third year].”
Enrollment Distribution. As noted, the current distribution of the uninsured population at the applicable income levels by state was used as a proxy for assigning each state a share of the national enrollment estimates generated by CMS. The underlying data used for the uninsured distribution were taken from “Table 3: Three-Year Average of Uninsured by Federal Poverty Level” in “Special Analysis: State Impact of Medicaid Eligibility Expansion,” produced by Federal Funds Information for States on April 23, 2009, which was in turn derived from the U.S. Census Bureau’s “Current Population Survey, 2008 (Uninsured data; three-year avg. 2005–2007).”
Federal Match Rates. Kaiser Family Foundation, StateHealthFacts.org data on FMAP rates by state for the five years FY 2005 through FY 2009 (using the pre-stimulus FMAPs for FY 2009) were averaged to produce a projected “baseline” or “normal” FMAP for future years for each state. These parameters were selected to exclude the otherwise distorting effects of the temporary FMAP increases in FY 2004 and post-stimulus FY 2009. The baseline FMAPs were then adjusted in accordance with the specific provisions of the legislation.
Administrative Cost Load. The administrative cost load was calculated using ratios for administrative spending to benefit spending and average federal and state shares of administrative costs, derived from the most recent actual data (FY 2006 and FY 2007) as reported in April Grady, “State Medicaid Program Administration: A Brief Overview,” Congressional Research Service Report for Congress, updated May 14, 2008, and John Holahan, Alshadye Yemane, and David Rousseau, “Medicaid Expenditures Increased By 5.3% in 2007, Led by Acute Care Spending Growth,” Kaiser Commission on Medicaid and the Uninsured, September 2009.



