The Affordable Care Act (ACA, also known as Obamacare) changed the individual insurance market in ways that altered the customer mix significantly, as well as the availability and design of insurance plans.REF Previously, the primary customers for individual market insurance were Americans who were either self-employed or buying coverage between jobs. They were mainly seeking financial protection for possible future medical expenses. After Obamacare, the primary customers became individuals seeking subsidized insurance to pay for their current medical expenses. That skewed the post-ACA individual market toward a risk pool consisting of older, less-healthy, and costlier-to-insure individuals.
In response to these changing market dynamics, insurers changed the design of their plans, including by charging patients higher deductibles and increasing plan out-of-pocket maximums.REF In many cases, insurers increased out-of-pocket limits on plans as high as the maximums allowed by the ACA ($7,350 for self-only coverage, and $14,700 for family coverage in 2018).REF
These changes are widespread throughout the Obamacare markets. More than half of all plan designs (54.7 percent) in the 39 states using the federally run exchange (Healthcare.gov) set out-of-pocket limits at the maximum allowed by the ACA.
Cost-sharing limits are set at the maximum level allowed in all Catastrophic-level plans; 51 percent of Bronze-level plan designs; 58 percent of Silver-level plan designs, and 41 percent of Gold-level plan designs.
One result: Numerous Obamacare plans now have out-of-pocket limits that are higher than the amount that the federal law allows in order for a plan to be paired with a health savings account (HSA). HSAs allow individuals to set aside money tax-free to pay medical costs. Consumers effectively get a discount on the cost of their medical care whenever they can avoid paying tax on the money used to purchase that care.
Congress specified that for a plan to be HSA-compatible, it must have a deductible that is no lower than the minimum set in law, and a limit on total out-of-pocket costs that is no higher than the maximum set in law. In 2018, the deductible must be at least $1,350 for self-only coverage or $2,700 for family coverage, and the annual out-of-pocket limit must not be greater than $6,650 for self-only coverage or $13,300 for family coverage.
Most Obamacare Plans’ Cost Sharing Is Too High to Be HSA-Compatible. Because Obamacare’s maximum out-of-pocket limits are higher than those for HSA-compatible plans, over half (57 percent) of all plan designs now offered on Healthcare.gov have out-of-pocket maximums that are too high for the plan to qualify as HSA-compatible. Only 30 percent of plans sold on the federal Obamacare exchange meet the criteria of having both a high-enough deductible and a low-enough out-of-pocket limit to qualify as HSA-compatible. Of the other, non-HSA-qualified plans, 19 percent do not qualify because their deductibles are too low, while 81 percent do not qualify because their out-of-pocket limits are too high.
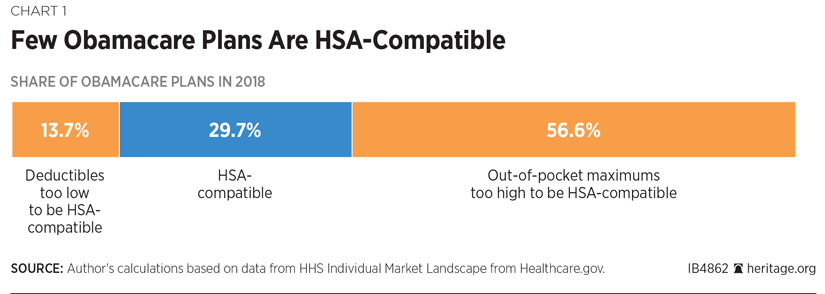
Most Obamacare HSA Plans’ Deductibles Are Higher than the Contribution Limit. Under most of Obamacare’s HSA-qualified plan designs, the enrollee cannot make a tax-free contribution to the account that would be large enough to cover the plan’s annual deductible. Of the HSA-qualified plan designs offered in the 39 Healthcare.gov states, 52 percent have deductibles for self-only coverage that are higher than the maximum allowable HSA contribution amount of $3,450, and 61 percent have deductibles for family coverage that are higher than the maximum allowable HSA contribution amount of $6,900. One-quarter of the HSA-qualified plan designs on Healthcare.gov have deductibles set at, or near, the maximum out-of-pocket limit.REF
In contrast, annual deductibles for workers with employer-sponsored HSA plans averaged $2,433 for self-only coverage, and $4,647 for family coverage in 2017.REF So, on average, workers in employer-sponsored HSA plans can cover their entire deductible with pre-tax contributions to their HSAs.
Under Obamacare, Insurers Are Constraining HSA-Plan Provider Networks. Insurers have also responded to escalating claims costs by narrowing provider networks. During the 2015 plan year, 54 percent of plan offerings had more restrictive networks, and by 2018 that figure has increased to 73 percent.REF HSA-qualified plans follow a similar pattern: 73 percent of HSA-qualified plans also have more restrictive networks this year. (See Chart 2.)

This constriction is something of an anomaly. Prior to Obamacare, insurers generally offered—and customers generally expected—a rough trade-off in plan design to provide customers value for their purchase. Typically, plans with higher out-of-pocket costs offered a broader choice of providers, while plans with limited provider choice offered lower out out-of-pocket costs. However, Obamacare has managed to force insurers into offering plans characterized by both limited provider choice and high out-of-pocket costs.
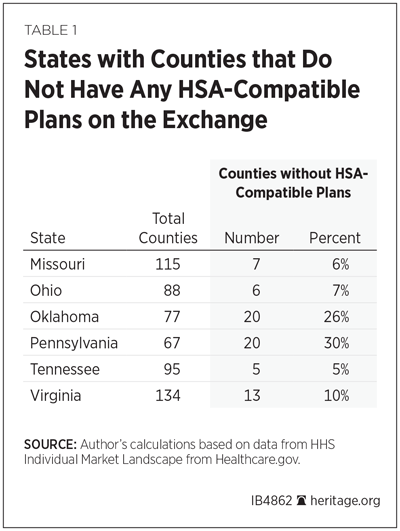
Some Obamacare Markets Have No HSA Plans. For the past three years, insurer choice and competition in the Obamacare exchanges have been shrinking—to the point that half of all U.S. counties now have only one insurer that offers exchange coverage.REF That diminished choice is also reflected at the plan level. This year, of the 39 states using Healthcare.gov, six have counties in which no HSA-qualified plans are available. (See Table 1.)
Solutions. Obamacare’s provisions are driving the disconnects discussed above. As with escalating premiums and narrowing provider networks, higher plan deductibles and out-of-pocket maximums are manifestations of the basic flaws in Obamacare’s public policy architecture. The only way to reverse that is for Congress to get back to work on repairing the damage done to the individual insurance market by Obamacare.
As part of that effort, Congress should expand individuals’ ability to choose a HSA-qualified plan by changing some statutory requirements. Proposals that might alleviate some of these issues include increasing tax-free contribution limits for HSAs to equal the maximum out-of-pocket limits.REF Another idea would be to define compatible coverage in terms of actuarial value instead of minimum deductibles and maximum out-of-pocket limits.REF In other words, rather than setting parameters for cost sharing, as the law currently does, plans could qualify as HSA-compatible if they covered no more than a specified percentage of the expected medical expenses of a statistically standard pool of enrollees. For instance, a plan with a 70 percent actuarial value is one that can be expected to pay 70 percent of the cost of covered benefits for a typical enrollee. So, the law could be changed to say that any plan with an actuarial value of, say, 70 percent or less, would qualify to be used with an HSA. Such a change would permit a wider range of plan designs to qualify as HSA-compatible.
Making America’s Health Care System Work for Patients
Americans’ health insurance choices have been narrowed under Obamacare. Addressing the problems outlined in this Issue Brief would be a good, incremental step to improve access to HSA-qualified plans that offer quality coverage. Further changes will be needed to fully empower patients, lower costs, and expand choices.
—Edmund F. Haislmaier is Preston A. Wells, Jr., Senior Research Fellow in Domestic Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation.

