Abstract: The military’s health care and retirement systems have serious structural problems. Simply tinkering around the edges will leave military personnel and taxpayers paying more for less service. Instead, as The Heritage Foundation proposes, Congress should transform the military health care and retirement systems into defined-contribution plans that maximize individual choice. This would enable military personnel to tailor their benefits to match their individual circumstances while saving the Department of Defense at least $39,424 million in five years.
The men and women who serve and have served in uniform and their families deserve quality health care and retirement benefits. U.S. service members should not be forced to choose between volunteering and quality health care.
Delivering first-class care, particularly in time of war, is a daunting challenge. Furthermore, care for military members, retirees, and their families should be portable. However, the Pentagon has built a system that is becoming increasing flawed. At a press conference on January 6, Secretary of Defense Robert Gates admitted that he had no solution for “the department’s unaffordable health costs, and in particular the benefits provided to working-age retirees under the TRICARE program.”[1]
While some argue that increasing military personnel’s contributions and scaling back military health and retirement in the existing systems would be sufficient, more substantial reforms are needed. The Department of Defense (DOD) outlined the increased contributions and reduced benefits approach in its fiscal year (FY) 2012 budget request.[2] As with other federal entitlement programs for health care and retirement, the military clearly cannot provide the promised benefits to its personnel and their dependents.
Pretending that the best approach is to preserve the existing military health care system is wrong. This “less of the same” approach is also an “all pain and no gain” approach for military service members and their families. There is a better way that would offset a portion of the future limits on health care and retirement benefits with selective increases in cash compensation.
This better way is to transform the military health care and retirement systems from the existing defined-benefit structures into a defined-contribution system. Under a defined-contribution approach, military service members and their families have much more flexibility to structure their health care and retirement in ways that best suit their preferences and needs. Ultimately, this approach makes the system fairer, more efficient, and less costly while preserving the military’s ability to recruit and retain high-quality personnel.
The Heritage Foundation’s fiscal plan Saving the American Dream would take exactly this approach. It would ensure continued recruitment and retention of top-quality personnel, honor the country’s obligations to members of its armed forces, and use taxpayer resources more efficiently and effectively to address veterans’ concerns and needs.[3] This systemic approach would also free resources for reinvestment in military modernization, which would achieve a better internal balance in the defense budget between the operational and modernization accounts. These reforms of the military health care and retirement systems could reasonably be expected to achieve at least $39,424 million in savings over five years.
The Need to Reform Military Benefits
The Heritage reform plan recognizes that the military provides health care coverage and retirement benefits inefficiently and corrects this by restructuring military health care and retirement coverage as defined-contribution plans as opposed to just tinkering with the existing defined-benefit plans. During the changeover to the new system, Congress will need to take into account the unique features of existing military health care and retirement coverage and tailor rules to smooth the transition from the existing structures to the new structures.
In Section 711 of the National Defense Authorization Act for Fiscal Year 2007, Congress recognized this problem in health care coverage and the implication that the military health care system is not sustainable.[4] This law established the DOD Task Force on the Future of Military Health Care.
The core problem is that the military health care system offers military personnel few options for obtaining health coverage that is tailored to meet their individual circumstances and preferences, and it provides little incentive for them to take responsibility for their own health care needs. As a general rule, a system that assumes that all of its participants have largely the same needs will inevitably be wasteful because it provides the range of benefits provided to everyone, whether or not they are needed or desired, while refusing to tailor coverage to individual preferences and needs. By providing health care more efficiently and by taking advantage of a whole-of-life approach to health coverage, tailored approaches can slow the growth in health care outlays by the Department of Defense while continuing to provide quality health care to service members and their dependents.
Congress has demonstrated less awareness of the inefficiencies in the military retirement system. It provides generous retirement benefits, but in a way that makes only relatively modest contributions to improving recruitment and morale. Its inflexible defined-benefit plan provides service members with few options for tailoring the system to their retirement preferences, particularly for employment beyond active-duty service.
The Military Health System
The Military Health System (MHS), also referred to as the Unified Medical Program, provides health care to more than 9.5 million beneficiaries worldwide, including active and Reserve military personnel, other uniformed services personnel,[5] military retirees, and their families.[6] The MHS cost nearly $49 billion in 2010 and employed 135,000 military and civilian personnel to provide health care services.[7]
The FY 2010 DOD report on TRICARE identifies four key mission elements for the program: “(1) maintaining Casualty Care and Humanitarian Assistance, (2) creating and sustaining a Healthy, Fit and Protected Force, (3) promoting Healthy and Resilient Individuals, Families and Communities, and (4) sustaining Education, Research and Performance Improvement.”[8]
This report also shows that MHS program costs have increased 14 percent in just three years, from $43 billion in 2007 to $48.9 billion in 2010, largely due to inflation and increased program utilization. The costs have also gone from 7 percent to 9.2 percent of the DOD budget. The Congressional Budget Office has projected that military medical spending will grow by more than 80 percent in real terms by 2024.[9]
The Saving the American Dream Plan
The Heritage Foundation’s Saving the American Dream plan provides tremendous advantages to the American people over the current systems for health care coverage and retirement. Among other advantages, it encourages Americans to build wealth, spurs economic growth, and puts the federal government’s financial house in order. Military service members and their dependents should have the same opportunity to benefit from these advantages that their civilian and private-sector peers enjoy. The plan achieves this through four major provisions: comprehensive tax reform, tax-deferred savings, a defined-contribution approach to Medicare, and a restructured Social Security program.
Provision #1: Tax Reform for Obtaining Family Health Coverage. The Heritage fiscal plan calls for comprehensive tax reform. It replaces the existing Byzantine tax code, including payroll taxes, with a simple flat tax system designed to collect up to 18.5 percent of gross domestic product (GDP). It also fundamentally changes how the federal tax code treats savings and expenditures for health coverage.
These latter provisions of the plan provide all Americans, including military service members and their dependents, with a full array of options for health care coverage. This system permits military service members to exercise greater control of their health care coverage and obtain the coverage that best suits their unique needs and preferences.
The Heritage plan accomplishes this by ending the existing tax exclusion for employee compensation in the form of employer-sponsored health insurance. This means that the value of employer-paid health insurance premiums is included in the employee’s total taxable compensation. Today’s system excludes employer-sponsored health insurance from income and payroll taxes, effectively giving upper-income workers in high-tax brackets a relatively large tax benefit.
The Heritage plan replaces the health insurance tax exclusion with a uniform, nonrefundable federal tax credit ($2,000 for an individual and $3,500 for a couple or family) to assist people in purchasing health insurance. Employers and employees decide whether the employer will continue to buy coverage or the employee will cash out the existing coverage in the form of higher cash income. Either way, the tax break for coverage is changed from an exclusion to a credit.
Under the Heritage plan, this credit can be used to offset the cost of coverage offered through the workplace or to buy insurance outside the workplace. For most middle-income working families, the value of the credit is similar to the tax relief that they receive from health insurance tax exclusion. The credit is advanceable, assignable, and available on a prorated basis. This means that the credit is available when premiums are due, enabling families to claim the credit for premiums paid before the end of the tax year. An assignable credit allows a family to assign their tax credit to a health plan in return for a dollar-for-dollar lower premium, eliminating the need to claim it on their own tax forms. Individuals and families with limited or no tax liability would receive direct financial assistance equivalent to the tax credit.
Provision #2: Tax-Deferred Savings for All Purposes Including Retirement. The basic structure of the Heritage tax plan is simple. With its single rate, it uniformly taxes all income sources that are spent on consumption. This means that taxable income includes all labor compensation and net borrowings. The amount put aside in savings, including for retirement, is then subtracted to determine net taxable income.
Thus, the more individuals or families save, the less they pay in taxes. Moreover, for tax purposes, it does not matter which goods or services are purchased, whether health care, education, retirement, or simple consumption goods. Further, the funds within these savings accounts may be transferred to heirs tax-free unless the heirs spend the money. Thus, the savings system permits tax-free intergenerational transfer of wealth.
Provision #3: Defined-Contribution Approach to Medicare. While the Heritage plan’s tax credit option for obtaining health care coverage provides lifetime advantages, including during retirement, Medicare remains in place for military retirees and their spouses. However, the plan recognizes the need to reform the existing Medicare system.
The Heritage plan accomplishes this by transforming Medicare from an open-ended and unsustainable defined-benefit entitlement into a properly budgeted program that focuses Medicare subsidies on those who need them most. The new Medicare program looks much more like the Federal Employees Health Benefits Program (FEHBP), the health care system for Members of Congress and federal civilian employees.[10]
Over a five-year period, the plan transforms Medicare into a defined-contribution system with stronger health security for the poor and less healthy and guarantees new protections against catastrophic costs for all enrollees. Today’s traditional fee-for-service Medicare program provides no protection against catastrophic costs. Because of this gap, 90 percent of seniors buy supplemental health coverage to protect themselves against the financial devastation of catastrophic illness. This means that seniors pay an extra set of premiums and often incur high out-of-pocket costs for both premium and non-premium medical expenses.
When the changes are fully phased in, seniors will enroll in the health plans of their choice and receive a defined contribution (premium support) toward the cost of their plans, much as Members of Congress and millions of federal civilian employees and retirees do through the FEHBP. Unlike today, all plans will include catastrophic protection. Thanks to the structure and insurance rules in Medicare, the premium support is sufficient for seniors to afford an adequate level of benefits, regardless of age or health care condition.
The range of choices in the transformed system includes Medicare premium-based fee-for-service insurance as well as other fee-for-service plans, Medicare Advantage plans, managed care plans, association plans, and Taft–Hartley Act and employer-based plans. Existing health savings accounts (HSAs) can also be carried into retirement.
Medicare’s basic rules for insurance are retained, together with an improved risk-adjustment mechanism to offset any adverse selection. Under the reformed system, Medicare’s Center for Drug and Health Plan Choice, which is tasked with identifying abuse and overseeing marketing rules for Medicare Advantage and Medicare drug plans, carries out that function for all plans in the transformed system.
Beyond retaining the Medicare insurance rules, the reform provides for fiscal solvency and reserve requirements for all health plans to ensure that plans have the financial resources to pay insurance claims. It also provides marketing rules to protect consumers against fraud and a requirement that benefits be described in plain English without surprises or denials in fine print. By increasing choice and competition, the reformed Medicare program delivers better care and provides true health care security for less money than under current projections.
The cash value of premium support is reduced for upper-income seniors and eventually phased out for those with the highest incomes. However, all seniors have access to the same Medicare system with no need to buy a separate plan to cover catastrophic expenses, and poor seniors would remain eligible for Medicaid assistance. Paralleling reforms in Social Security in the Heritage plan, Medicare’s eligibility age is increased to 68 in 10 years and is indexed thereafter for increases in longevity.
During the five-year transition period, Medicare’s traditional fee-for-service system also changes. A new premium payment system for upper-income retirees would offset Part A costs. The premiums for Parts B and D rise according to income. The highest-income seniors pay an unsubsidized premium for Parts B and D during the transition.
Provision #4: Ensuring That Social Security Provides Protection Against Poverty. As with Medicare, the Heritage plan restructures Social Security to preserve it for future retirees, including future military retirees. The centerpiece of the new Social Security system involves a gradual transition to a flat benefit that pays workers who qualify for a full Social Security check. This amount is well above the income level that the Census Bureau says an American over the age of 65 needs to avoid poverty.
Thus, the new system guarantees that no retiree falls into poverty because of insufficient income and ensures a reasonable income for seniors. Under today’s system, workers can pay Social Security taxes for 35 years and still receive a benefit that is below the poverty level, forcing some workers to go on welfare. The new system corrects this serious flaw.
The flat benefit is the equivalent of about $1,200 per month in 2010 dollars when the reform is complete. This is both higher than today’s average Social Security retirement benefit payment ($1,164 per month) and well above the 2009 poverty level for a single adult over age 65 ($857 per month). To ensure that future retirees do not slip back into poverty, the flat benefit level is indexed for wage growth.
The Transition to the New Plan
While the Saving the American Dream plan applies to all Americans, the existing health care and retirement systems for military service members and their dependents are quite different from those for other Americans. Accordingly, an orderly transition from the existing systems to the new ones will require making careful arrangements to phase out TRICARE and the military retirement systems.
Transforming Military Health Care. The transition to the new health care system for service members and their dependents:
- Allows current service members and their dependents to continue with TRICARE.
- Allows service members to purchase insurance through the FEHBP. Current service members who opt for the new system, new recruits, and their dependents are provided access to private health insurance services through the FEHBP.[11] Alternatively, they can choose to buy insurance outside the FEHBP.
- Increases service member pay to compensate for foregone TRICARE benefits. Service members under the new system receive a significant pay increase in lieu of the health care benefits they would otherwise have received under TRICARE.
- Enables MHS and the Veterans Affairs system to specialize in military medicine. The MHS network and the Veterans Affairs system continue to provide medical services to eligible and enrolled former service members. This enables them to specialize even more in military medicine and in meeting the unique medical needs of former service members with service-related injuries or diseases.
Continuing TRICARE for Current Service Members and Dependents. Such a far-reaching change in health coverage system for service members and their dependents cannot take place overnight, nor should it. All new recruits enter under the new system, but current members can choose to continue with TRICARE or to enter the new system. Relatively young service members are more likely to choose the new system. As new recruits replace current members, TRICARE gradually phases out.
Leveraging Private Health Insurance. The Heritage plan provides access to private health insurance services to military service members and their dependents through the FEHBP, the same system used by federal civil servants. Premiums for the insurance coverage vary according to the specific plans, and the federal government, as the employer, and the civil servant make payments to cover the premiums.
However, the FEHBP system as applied to military service members and their dependents differs from what is offered to civil servants in two critical ways. First, the service member pays the entire premium in accordance with the Heritage fiscal plan because the tax preferences are transferred from the employer to the individual. Second, a service member is free to buy insurance outside the FEHBP.
A Significant Pay Increase. Under the new system, service members in the new system no longer receive health care benefits under TRICARE and are responsible for paying for health insurance for themselves and their dependents, including premiums and cost sharing. Accordingly, they receive higher gross pay than their colleagues who remain under TRICARE.
According to the Congressional Budget Office, the Department of Defense paid roughly $3,000 in health care costs per person for service members and their dependents in 2007.[12] To maintain an internally balanced defense budget, the DOD must reduce per capita costs. Therefore, the pay increase for service members in the new system must be less than $3,000 per person. Furthermore, the increased efficiency of the new health care system cannot justify this level of pay increase.
On this basis, the Heritage plan recommends increasing the cash pay for service members by 2 percent above any general pay increases provided to colleagues of similar rank and time of service who remain under TRICARE. This creates a two-tiered pay system in the military for a time, but it eventually disappears as service members retire.
Focusing on Military Medicine. The MHS is a network of 59 hospitals and 364 clinics that operate under the Department of Defense to provide a wide array of health services to service members, former service members, and their family members.[13] The MHS mandate is overly broad, but the new system of health care coverage narrows this mandate to allow the MHS to focus more on meeting the unique needs of military medicine and less on providing a broad range of medical services to former and current service members and their dependents.
The Heritage plan anticipates that all active-duty service members, including Reserve personnel on active service, retain the option of using the MHS free of charge. They also retain the option of seeking medical services outside the MHS, for which they could pay directly through their private insurance plan or through a combination of the MHS and private insurance. In this context, the private insurance company would offer insurance plans through the FEHBP that are tailored to active-duty service members who have access to the MHS while on active duty.
With private health care coverage providing medical services to dependents and routine care to service members, the MHS could specialize in military medicine and make its hospitals and clinics centers of excellence in providing this kind of care. For example, MHS facilities would care for a service member who is wounded in battle or needs vaccinations for deployment to a particular theater of operation. However, for more routine medical services and those that are less related to military medicine, the service member’s best care option would likely be outside the MHS. While a service member’s primary incentive for carrying private insurance is to have insurance after active-duty military service, he or she will have the additional incentive to carry it for greater access to superior care outside the MHS while still on active duty.
The Reserve component personnel not on active duty retain access to the MHS, but not free of charge. In this case, the MHS hospital or clinic would charge rates equivalent to rates for the same service provided in a civilian hospital or clinic. The reservists would depend on private insurance or direct payments to cover these costs. In all likelihood, these service members would tend to use civilian hospitals or clinics.
In contrast to the current system, the qualifying dependents of military personnel cannot access the MHS system unless they are accompanying the service member to hardship posts where access to health care services outside the MHS is unreliable. As with Reserve component personnel, these services are subject to fees at rates equivalent to those charged by civilian service providers, and the cost of services is covered by the private insurance plans and out-of-pocket payments.
The VA offers a wide range of medical services to eligible and enrolled former service members through a network of more than 1,400 hospitals and clinics.[14] Because VA facilities and services are not funded through the defense budget, they are not the focus of this paper. Nevertheless, the health coverage provided to service members through the Department of Defense under the Heritage plan would affect VA operations because it is designed to be available to the service member for life. In this context, it should permit the VA and the MHS to focus on meeting the unique medical needs of former service members with service-connected injuries or diseases.
Transforming the Military Retirement System. Much like the transition to the new health care system, the transition to the new military retirement system:
- Allows current military personnel to retire under the existing retirement system. The Heritage plan replaces the existing defined-benefit structure for military retirement with a defined-contribution plan. Accordingly, no service member who is already in the military and has planned for his career, both in the military and beyond, on the basis of the existing retirement system should have it taken away. Thus, he or she has the option of continuing with the current system or joining the new one.
- Provides special pay and bonuses that are earmarked for retirement accounts. To maximize recruitment and retention under the new system, the military should be free to offer incentive payments to service members as long as the member commits to contributing the designated special pay and bonuses to his retirement account. For example, the military could offer a long-term bonus package for contribution to a service member’s retirement account to encourage the member to make a full career of the military. On the other hand, a more immediate bonus package could encourage a prospective recruit to enlist for a shorter time.
- Gradually expands the Thrift Savings Plan (TSP). The savings options provided under the Heritage plan, in essence, are an expanded version of the existing TSP.
- Adjusts existing retirement benefits for inflation. The Heritage plan’s proposal for Social Security changes how Social Security benefits are adjusted for inflation because cost-of-living adjustments (COLAs) do not accurately reflect the impact of inflation on retirees. Benefits for military retirees are currently adjusted on a similar basis as Social Security benefits using the Consumer Price Index (CPI). This transition arrangement preserves this link[15] and means that future military retirees are covered under the existing defined-benefit structure in which COLAs are based on the more accurate Chained Consumer Price Index (C-CPI-U).
- Provides disability retirement coverage through the VA and, if necessary, a reformed Social Security system . The Heritage plan eliminates the existing disability military retirement for new entrants but reforms Social Security, including its disability system, and new recruits would have access to this system. Specifically, the plan recognizes that some workers, including disabled service members, are physically unable to work until retirement age. It therefore includes an improved disability system to ensure that those who are unable to work receive a quick and accurate decision on their benefit application rather than facing today’s long delays. It also improves today’s often arbitrary decision-making process. Disability retirement has an accrual cost of less than 1 percent of basic pay. This amount should be easily offset by enhancing VA programs if required.
Cost Savings to the National Security Account
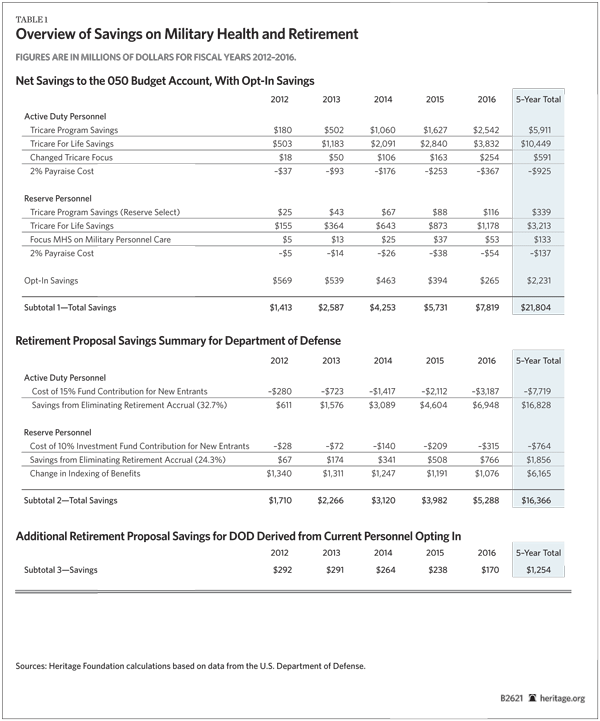
The Heritage proposals to reform military health care coverage and retirement will produce substantial net savings to the national security account (050) in the federal budget.[16] However, the level of savings cannot be calculated precisely because of the grandfathering of existing elements to allow current military personnel to choose between joining the new plans and keeping their existing coverage. Nevertheless, it is possible to calculate the base level of savings with new recruits.
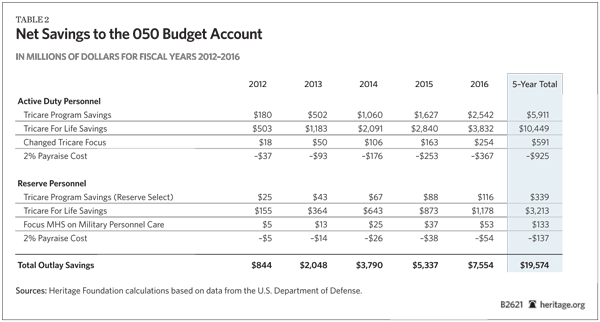
Health Care Coverage Savings. Applying the Saving the American Dream plan to new recruits would save almost $20 billion[17] over the five years from FY 2012 through FY 2016 from the four elements of the reform proposal:
- TRICARE savings. These savings result from replacing TRICARE for new recruits and their dependents. This element saves an estimated $6 billion from the active component and $339 million from the Reserve component over five years.
- TRICARE for Life savings. Eliminating the accrual payments for future TRICARE benefits for current personnel who retire and become Medicare recipients saves somewhat less than $10.5 billion over five years from the active component and slightly more than $3.2 billion from the Reserve component.. Rather than TRICARE, military veterans participate in the new defined-contribution Medicare plan for all Americans.
- Changed focus for the military health care system. Permitting the military health care system to focus on military medicine saves almost $600 million from the active component and a little more than $130 million from the Reserve component.
- Increased outlays for the selective pay increase. The 2 percent pay increase to participating service members partially offsets the gross savings to the budget account. Over five years, the pay increases are expected to cost more than $900 million for the active component and almost $140 million for the Reserve component.
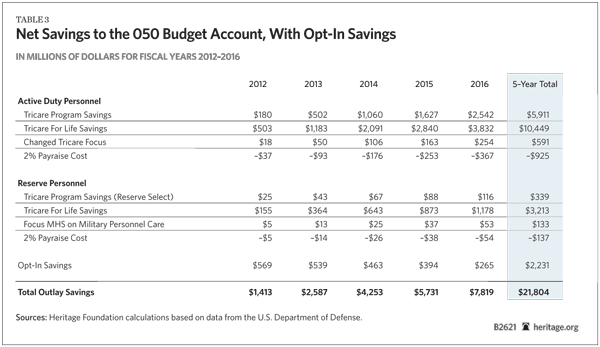
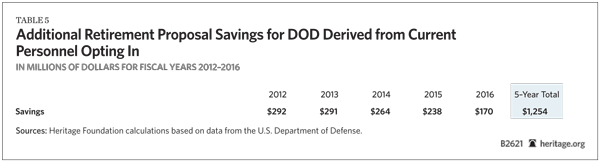
Applying the same four elements of the reform proposal to current military personnel produces additional savings, although the exact level will depend on how many of them choose the new plan over TRICARE. Assuming that 10 percent of currently serving military personnel with six or fewer years of service choose the new plan in FY 2012, the DOD would save a total of nearly $22 billion. (See Table 2.)
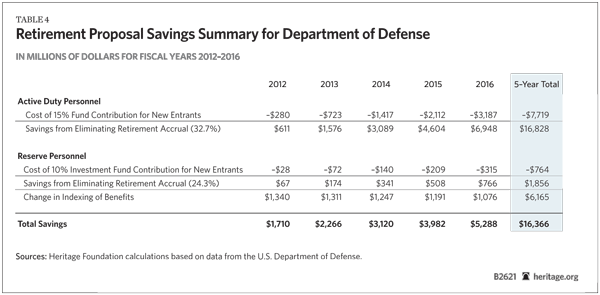
Retirement Savings. DOD savings from the recommended reforms for the military retirement system can be calculated in a similar manner. If only future recruits are brought into the proposed systems, the DOD would save $16 billion over five years. (See Table 3.) However, a significant number of younger service members may opt into the new system. If only 10 percent of currently serving military personnel with six or fewer years of service opt into the new system in FY 2012, the DOD could save an additional $1.2 billion over five years. (See Table 4.)
In addition, adjusting retirement annuities with the Chained CPI achieves additional savings from service members who are not participating in the new system. Because this covers the large majority of service members, the savings will be significant.
Impact on Retention Rates
Such a significant change in compensation could affect personnel retention. However, because this proposal applies only to new entrants and other personnel who voluntarily opt in and because the DOD has extreme flexibility in determining payments to individuals, any such impacts are expected to be minimal.
On the other hand, the more flexible retirement system gives the military a powerful tool that allows it to direct retirement compensation in ways that will actually improve recruitment and retention. For example, recruitment for positions that assume short-term careers in the military could be enhanced by providing special pay and bonuses that are earmarked for retirement account contributions by the member shortly following recruitment, such as between two years and four years into the service period. The military could improve retention in longer-term specialties by providing earmarked special pay and bonuses that require longer military careers, such as after 15 or 20 years of service.
Conclusion
Trying to save money by tinkering around the edges of the Military Health System and the military retirement system is unwise because both systems have serious structural problems. These problems mean that the current system does not serve the best interests of either military members and their dependents or taxpayers. First, these systems do not allow military service members and their dependents to take responsibility for their health care and retirement by tailoring their coverage to their preferences. Second, this same inflexibility leads to inefficient use of scarce defense funding, which is a disservice to taxpayers.
However, systemic reform of the Military Health System and military retirement system can give military service members and their dependents the ability and financial means to chose coverage plans that best meet their preferences. With the recommended reforms, fewer taxpayers’ dollars will purchase more health care and retirement benefits for service members and their dependents. The key to these reforms is to replace existing systems with new systems that treat service members and their dependents as individuals with individual health care needs and preferences rather than as members of a class with identical needs and preferences.
—Baker Spring is F. M. Kirby Research Fellow in National Security Policy in the Douglas and Sarah Allison Center for Foreign Policy Studies, a division of the Kathryn and Shelby Cullom Davis Institute for International Studies, at The Heritage Foundation.
Appendix A
Summary of TRICARE
TRICARE is a group of medical care options for military personnel, military retirees, and their families. This section summarizes the major options available under the system.
TRICARE Prime. TRICARE Prime is the principal component of this system. It is essentially a DOD-run health maintenance organization that provides medical care to military personnel and their dependents. Care is generally provided in Military Treatment Facilities as well as by affiliated civilian facilities and providers. Enrollment in TRICARE Prime is required for active-duty service members, including Reserve personnel on active duty under federal orders for more than 30 days. Enrollment is optional for family members of active-duty personnel, who are also eligible for TRICARE Standard and TRICARE Extra. TRICARE Prime charges no premiums to active-duty service members or their family members. However, participating military retirees pay co-pays for most services.
TRICARE Standard and TRICARE Extra. TRICARE Standard is the military equivalent of a health insurance plan for active-duty family members and military retirees and their dependents. Participants have an annual deductible and co-payments but no premiums. TRICARE Standard provides participants with greater health care choices than are available under TRICARE Prime. TRICARE Extra is similar to TRICARE Standard except that beneficiaries’ co-pays are reduced when they use designated network providers.
TRICARE Reserve Select. TRICARE Reserve Select is a premium-based plan available to selected Reserve personnel and their families. (Reservists injured or sickened in the line of duty receive free line-of-duty care for their needs.) Coverage is similar to TRICARE Standard and TRICARE Extra. Reservists enrolled in or eligible to participate in the FEHBP may not participate in TRICARE Reserve Select. The government subsidy for TRICARE Reserve Select is set at 72 percent, the same as the subsidy for the FEHBP.
TRICARE Retired Reserve. TRICARE Retired Reserve is a premium-based plan for retired Reserve members who have qualified for Reserve retirement but have not reached the age requirement (age 60) for a retirement annuity. (This group is commonly referred to as “gray area” retirees.) Personnel eligible for the FEHBP cannot participate in this program. Rates are quite high (nearly $1,000 per month for the member and family in 2010) because there is no government subsidy for this program. After reaching age 60, eligibility ends, and retired Reserve members may participate in TRICARE Prime, Standard, or Extra.
TRICARE for Life (TFL). TFL provides additional coverage for TRICARE beneficiaries, regardless of age, who also have Medicare Part A and Part B coverage. TFL acts as a secondary payer and reduces beneficiaries’ out-of-pocket expenses.
Transitional Assistance Management Program (TAMP). TAMP provides transitional health care benefits to certain personnel separating from federal active duty, including active-duty personnel involuntarily honorably separated from duty, Reserve component personnel separating after at least 30 days active duty in support of a contingency operation, personnel separating from active duty after being retained under “stop-loss” for a contingency operation, personnel separating from active duty after voluntarily staying on active duty for less than one year in support of a contingency operation, and personnel separating from active duty to become a Selected Reserve member without a break in service. TAMP provides health benefits for 180 days under the same rules for regular active-duty personnel and family members. After TAMP benefits expire, a premium-based Continued Health Care Benefit program can provide up to 36 months of coverage.
TRICARE Benefit Examples
Example 1: A service member who serves one tour on active duty and then pursues a civilian career. During active duty, the member is required to enroll in TRICARE Prime. The service member’s family can use TRICARE Prime, Standard, or Extra. Upon leaving the service, neither the service member nor the family is eligible for further TRICARE benefits unless the service member falls into one of the categories of eligibility for TAMP benefits, which provides time-limited eligibility for continued TRICARE benefits.
Example 2A: A service member who serves 10 years on active duty and then transfers to a Reserve component as a Selected Reserve member. While on active duty, enrollment options are the same as in Example 1. A member who transfers immediately to a Reserve component is eligible for TAMP TRICARE benefits for 180 days. During or after that period, if not FEHBP-eligible, the member can enroll in TRICARE Reserve Select for continued TRICARE benefits after TAMP coverage ends.[18]
Example 2B: A service member who retires from active duty and then transfers to a Reserve component as a Selected Reserve member. While on active duty, enrollment options are the same as in Example 1. As a military retiree, the member maintains TRICARE eligibility and may participate in TRICARE Prime, Standard, or Extra. Because the member has other TRICARE coverage, he or she is not eligible for TRICARE Reserve Select.
Example 3: A Reservist and a National Guard member activated for federal service. All Reserve component personnel activated for 30 days or more must participate in TRICARE Prime. If activated for less than 30 days, they continue their relevant TRICARE eligibility. Over half of the states provide continuation of health and life insurance benefits for activated National Guard members who are also state employees, allowing family members to continue any state health benefit coverage. A few states provide assistance with private insurance.[19]
Appendix B
The Existing Military Retirement System
The military retirement system has several components.
Defined Benefits. The military retirement system provides non-disability, survivor, and disability payments to eligible persons. In 2009, it provided $51.1 billion in benefits to 2.2 million retirees and survivors. The system is accrual-funded, which means that DOD pays the expected cost of retirement benefits for its personnel via contributions to the Military Retirement Trust Fund as a percentage of their basic pay. Military personnel make no direct contribution to fund their retirement benefits. Eligibility for immediate non-disability retirement pay requires a minimum of 20 years of service at any age. Reserve retirement generally requires 20 qualifying years of service, and benefits are based on a point system for drills and active-duty training and service, but retirement pay commences at age 60. A minimum of 50 points earned annually qualifies as a year that is creditable for Reserve retirement, whereas 360 points equals a full year of service in calculating the retirement annuity. Public Law 110–181 allows a 90-day reduction in the Reserve retirement age of 60 for every three months served in a contingency operation after its enactment.
A “Cliff Vested” System. Military retirement is a cliff-vested system because there is no vesting prior to 20 years of service for non-disability retirees. Disability retirement requires that the disability not be the result of the member’s intentional misconduct or willful neglect or have been incurred during an unauthorized absence. It also requires a disability rating of at least 30 percent on the VA rating scale and one of four other conditions, such as a disability that resulted from active duty.
Three Non-Disability Benefit Formulas. Three non-disability retirement benefit formulas apply to active-duty military personnel, depending on when they entered the military.
- Personnel who first entered the military before September 8, 1980, receive retired pay equal to final basic pay times 2.5 percent for each year of service.[20]
- For personnel who first entered service after September 8, 1980, and before August 1, 1986, the average of the highest three years of basic pay (Hi-3) is used to calculate annuities rather than final basic pay. This group accounts for an estimated 3.8 percent of personnel on the total basic payroll.
- Personnel who entered the military on or after August 1, 1986, choose between the Hi-3 retirement annuity formula or a reduced annuity formula (Redux) in combination with a $30,000 Career Status Bonus (CSB). The Redux annuity calculation includes lower multipliers for members retiring with less then 30 years of service. However, at age 62, retired pay is recomputed with the regular 2.5 percent multiplier. The CSB is paid at 15 years of service as a lump-sum or in installments. Members who serve less than 20 years forfeit part of the $30,000 CSB.
Inflation-Adjusted Benefits. Military retirement and survivor annuities are adjusted annually for inflation using the CPI. Retirees who entered the military before August 1, 1986, or who do not opt for Redux/CSB receive adjustments equal to the CPI increases. Those who opt for Redux/CSB receive adjustments equal to the CPI minus 1 percent for life (except when the CPI is 1 percent or less), with an annuity recomputation to a full CPI at age 62.
VA Compensation. In addition to military disability and non-disability retirement benefits, veterans may be eligible for compensation for certain disabilities through the VA. Historically, veterans compensation has been offset against any disability or non-disability retired pay because the payments result from the same military service. Members benefit more from VA benefits than they do from military retirement benefits because VA payments are exempt from federal income taxes. However, beginning in 2004, the offset has been steadily reduced by Congress to allow at least partial receipt of both military retirement and VA compensation. This is commonly referred to as “concurrent receipt.” The major significance of concurrent receipt for this analysis is that its cost is reflected in the accrual payments for military retirement. However, the Treasury, not the DOD, pays these costs. Thus, they are not covered in this paper.
“Normal Cost” Payment System for DOD. As noted earlier, the DOD pays the accrual or “normal cost” as a percent of basic pay (NCP) for retirement benefits for military personnel, except for the concurrent receipt cost. For active-duty personnel under Hi-3 and CSB/REDUX, the total weighted NCP is 32.7 percent for 2010. Of this, 30.9 percent is for non-disability benefits, 0.6 percent is for disability benefits, and 1.2 percent is for survivor benefits. For reservists (part-time personnel), the corresponding NCPs are 22.6 percent, 0 percent, and 1.7 percent. Therefore, relatively little funding goes to disability and survivor benefits.
The Thrift Savings Plan. Military personnel also participate in the federal Thrift Savings Plan, a tax-deferred retirement savings plan originally limited to federal civilian employees, which operates much like 401(k) plans. Members may contribute any percentage of basic, special, and incentive pay and bonuses on a pre-tax basis up to a limit of $16,500 for 2010—the same limit on 401(k) plans. Unlike federal employees covered by the Federal Employees Retirement System, the DOD generally does not match service members’ contributions to their TSP accounts. The DOD has authority to match for critical occupations in exchange for a service commitment, but it is not currently using this authority. The Army had a TSP matching pilot program for new recruits in certain critical specialties that ran from 2006 through 2008. TSP funds are available to members for in-service loans without tax penalty to purchase general and primary residences.
TSP participants choose to invest in up to six different investment funds: the Government Securities Investment (G) Fund; Fixed Income Index Investment (F) Fund; Common Stock Index Investment (C) Fund; Small Capitalization Stock Index Investment (S) Fund; International Stock Index Investment (I) Fund; and Lifecycle (L) Fund. The Lifecycle Fund is a mix of the other five funds, designed to optimize returns based on a target retirement date and risk level. For example, participants further away from retirement can tolerate more risk in pursuit of higher returns, so a greater percentage of their assets is invested in the riskier funds such as the C, I, and S Funds. For a given risk level and time horizon, the L fund seeks an optimal mix of the G, F, C, S, and I Funds to provide the highest return. The G Fund is risk-free because the securities are backed by the U.S. government.
The TSP will add a Roth 401(k) feature in 2011, as authorized in recent legislation. Contributions would be made from after-tax income, but earnings and withdrawals at or after age 59.5 would be tax-exempt.
Examples Under the Current System for Active-Duty Members
Example #1: An active-duty member. An active-duty member must serve a minimum of 20 years to qualify for an immediate lifetime annuity for non-disability retirement. (Disability retirement applies to those who are disabled as a result of service.) New personnel choose between a retirement annuity of 2.5 percent for each year of service based on Hi-3 or Redux for pre–30 years of service retirement combined with a $30,000 Career Status Bonus (CSB). At age 62, Redux recipients’ retired pay is recomputed with the regular 2.5 percent multiplier. Hi-3 retirees receive adjustments equal to the CPI increases. Redux/CSB retirees receive adjustments equal to the CPI minus 1 percent for life (except when the CPI is 1 percent or less), with an annuity recomputation to a full CPI at age 62.
Example #2: A Reservist. Reserve retirement benefits are similar to those for active-duty personnel retiring under Hi-3 except that benefits generally commence at age 60 and are reduced proportionately using the points system to account for the part-time nature of Reserve service. A reservist must serve 20 creditable years to qualify for a retirement annuity. Any year in which the member earns at least 50 points through drills, active duty for training, and active duty is a creditable year, whereas 360 points equals a full year of service in calculating the retirement annuity. Thus, a reservist earning the 50-point minimum for 20 years receives a retirement annuity of 50/360of the active-duty calculation. Reserve retirees also receive full CPI adjustments annually.