During 2015, the growth in both individual-market and employer-group coverage resulted in a net increase in private-market coverage of 2 million individuals. For individual-market policies, enrollment increased by a bit more than 1.12 million individuals.[1] For the employer-group-coverage market, enrollment in fully insured plans declined by 932,000 individuals, while enrollment in self-insured plans increased by 1.86 million individuals.[2] The net effect of those changes was an increase of 926,000 in the number of individuals with employer-sponsored coverage in 2015.
Public program enrollment in Medicaid and the Children’s Health Insurance Program (CHIP) increased by almost 2.77 million individuals in 2015. As in 2014, the change in Medicaid enrollment in 2015 differed notably between states that adopted the ACA’s Medicaid expansion and states that did not. States with the ACA’s Medicaid expansion in effect experienced Medicaid enrollment growth of almost 2.13 million people, while in the states without the expansion in effect, Medicaid enrollment grew by 640,000 individuals.
Thus, the net changes in private and public enrollment combined resulted in a little more than 4.8 million individuals gaining coverage during 2015. Roughly two-fifths of that increase occurred in the private market, and three-fifths occurred in Medicaid.
Two Years’ Enrollment Experience
For the two-year period 2014 and 2015, enrollment in individual-market policies increased by 5.9 million individuals, from 11.8 million at the end of 2013 to almost 17.7 million at the end of 2015.
For the employer-group coverage market, enrollment in fully insured plans dropped by 7.6 million individuals, from 60.6 million at the end of 2013 to 53 million as of the end of 2015. During the same two years, enrollment in self-insured employer plans increased by 4 million individuals, from 100.6 million in 2013 to 104.6 million in 2015.
The combined effect of the changes in individual-market and employer-group coverage was a net increase in private-sector coverage of 2.3 million individuals during the two-year period.
Net Medicaid and CHIP enrollment over the two years grew by almost 12 million individuals, from 60.9 million at the end of 2013 to 72.7 million at the end of 2015. In states that adopted the ACA Medicaid expansion, enrollment increased by 10.4 million; in states that did not adopt the expansion, enrollment increased by 1.4 million individuals.
Thus, for the two-year period, the combined enrollment increase in both private and public coverage was just over 14 million individuals—with 84 percent of that increase attributable to the ACA Medicaid expansion.
Diminishing ACA Effects
The Department of Health and Human Services (HHS) reported that as of the end of 2015, 8,780,545 people were covered by individual-market plans purchased through ACA exchanges, of which 7,375,489 received subsidies that offset the cost of their coverage.[3] Thus, of the 17.7 million people with individual-market coverage (both on and off the exchanges) as of the end of 2015, about 7.4 million (42 percent) had their coverage subsidized by taxpayers, and the remaining 10.3 million (58 percent) paid the full cost on their own.
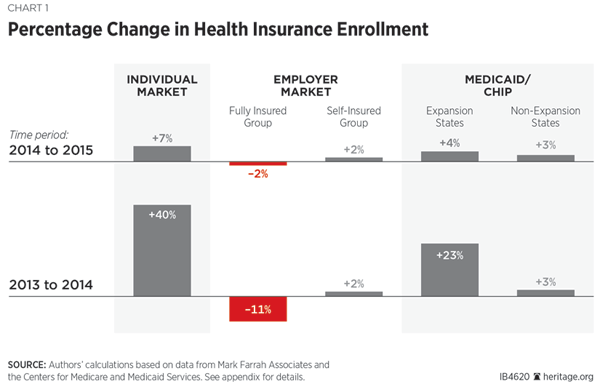
As Chart 1 shows, three coverage segments experienced significant change in 2014, but in all three the rate of change diminished considerably in 2015. Enrollment in the individual market grew by 40 percent in 2014 and by an additional 7 percent in 2015. Enrollment in fully insured employer-group plans declined by 11 percent in 2014 and by a further 2 percent in 2015. For the states that adopted the ACA Medicaid expansion, Medicaid and CHIP enrollment increased by 23 percent in 2014 and by 4 percent in 2015. Three states (Alaska, Indiana, and Pennsylvania) implemented the Medicaid expansion in 2015, and Medicaid enrollment growth in those states accounted for 28 percent of all expansion-state Medicaid enrollment growth in 2015 (or just over 1 percentage point of the 4 percentage point growth in expansion states).
In contrast, the number of individuals covered by self-insured employer plans grew by 2 percent in both years. Similarly, Medicaid enrollment grew by 3 percent in both years in states not implementing the Medicaid expansion.
Conclusion
Implementation of the ACA appears to have had three effects on insurance coverage: a substantial increase in individual-market enrollment, an offsetting decline in fully insured employer-group plan enrollment, and a significant increase in Medicaid enrollment in states that adopted the ACA Medicaid expansion. In all three cases, those effects were greatest in 2014 and continued, though at much reduced rates, in 2015.
—Edmund F. Haislmaier is Senior Research Fellow in the Center for Health Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation. Drew Gonshorowski is Senior Policy Analyst in the Center for Data Analysis, of the Institute for Economic Freedom and Opportunity, at The Heritage Foundation.
Appendix
Data Sources and Adjustments
We used the Mark Farrah Associates dataset, derived from insurer regulatory filings compiled by the National Association of Insurance Commissioners (NAIC), for private-market enrollment by market segment. We excluded as not relevant to our analysis enrollments in Federal Employees Health Benefit plans, Medicare Advantage plans, and supplemental coverage products (such as dental, vision, prescription drug, Medicare supplemental, and single disease).
For enrollment in self-insured employer plans, we used the data reported by Mark Farrah Associates for plans administered by an insurance carrier. Mark Farrah compiles these data from insurer regulatory filings, supplemented by other public and private sources such as Securities and Exchange Commission filings. While the firm’s data on the self-insured market are the most comprehensive available, there are no reliable figures for enrollment in self-insured plans that are administered by independent third-party administrators (TPAs)—that is, TPAs that are not subsidiaries of insurance carriers. However, based on its research, Mark Farrah Associates believes that truly independent TPAs likely account for no more than 5 percent of the total self-insured market.[4]
For Medicaid and CHIP enrollment, we used the figures from CMS state-level monthly enrollment reports as they include enrollment under both Medicaid fee-for-service and Medicaid managed-care plans and are “point-in-time” counts, which makes them consistent with the “point-in-time” counts of private-market coverage in insurer regulatory filings.[5] The CMS reports do not include enrollment data for December 2013, but we were able to obtain those figures from a report by the Kaiser Commission on Medicaid and the Uninsured and used them as the basis for calculating enrollment growth during 2014.[6]
We made several adjustments to the Mark Farrah Associates private-market data to make them as complete and accurate as possible. Specifically:
- Arkansas implemented the Medicaid expansion through a so-called private-option design. Under that approach, qualified individuals are enrolled in the state’s Medicaid program and then, at the beginning of the month following enrollment, select (or are assigned) coverage through a Silver-level plan offered in the exchange, with Medicaid paying almost all of the premiums. This arrangement could result in double counting those individuals in our analysis. The CMS Medicaid enrollment reports include private-option enrollees in Arkansas’s Medicaid enrollment figures. However, the regulatory filings by carriers offering exchange coverage in Arkansas include private-option enrollees in their enrollment counts for individual-market coverage—which, from the carrier perspective, would be appropriate. Separately, the Arkansas Department of Human Services (DHS) reported that the number of individuals with completed private-option enrollment at the end of 2015 was 200,703.[7]
- Consequently, to avoid counting private-option enrollees twice, we subtracted the Arkansas DHS figures from the figures for total individual-market enrollment for Arkansas derived from the insurer regulatory filings. Thus, our analysis counts Arkansas private-option enrollees as Medicaid enrollees.
- Data for one California carrier were missing from the Mark Farrah Associates dataset, but we were able to obtain the carrier’s enrollment figures from the report it filed with the California Department of Managed Health Care.
- Four New York carriers that offer coverage through that state’s exchange are Medicaid managed-care insurers that did not offer coverage in the individual or group markets before 2014 and do not file NAIC reports, as they are regulated by the New York State Department of Health. For those carriers, we used the figures from the 2015 enrollment report published by the state exchange.[8] However, we were able to obtain enrollment numbers for those carriers for the end of 2014 from their federal medical loss ratio (MLR) report filings and updated our 2014 figures accordingly.
- Finally, three insurers that were put into insolvency proceedings by state regulators did not file fourth-quarter reports. We used the enrollment figures reported by those carriers on their most recent (third quarter 2015) NAIC filings on the presumption that most, if not all, of those enrollees still had their coverage in force through the end of 2015.
The net effects of the foregoing adjustments to the enrollment figures derived from the Mark Farrah Associates dataset were increases of 58,191 for the individual market and 29,903 for the fully insured group market.